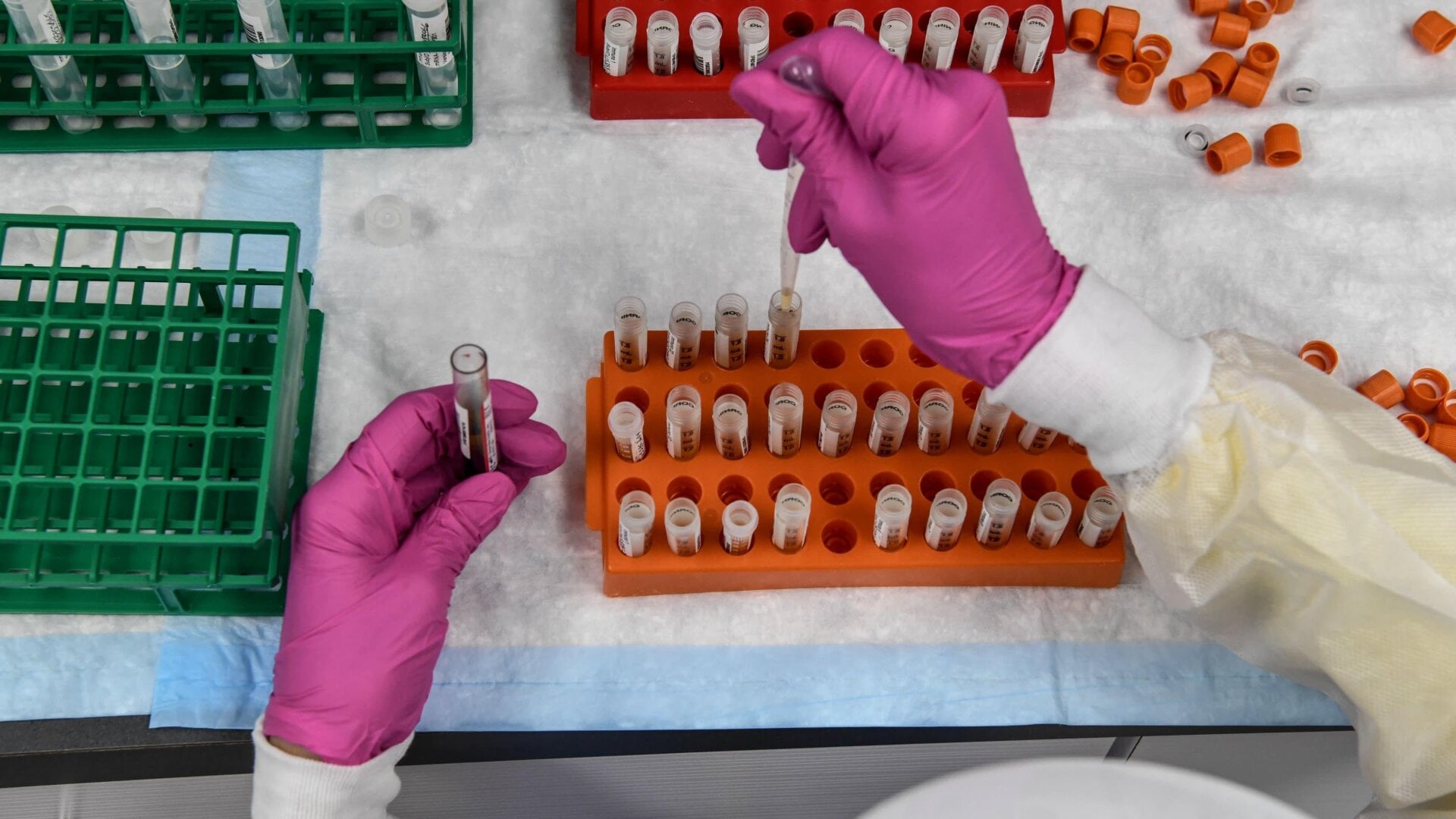
A vaccine for the coronavirus that causes covid-19 appears to be our best strategy to ending the current pandemic. Unfortunately, the fastest time frame in which scientists have managed to create any vaccine in history was four years, and there’s already plenty of skepticism surrounding the safety, availability, and effectiveness of any future covid-19 inoculation. So let’s go over the most pressing questions.
When could it be ready?
Scientists around the world have collectively made leaps and bounds in developing potential vaccines against SARS-CoV-2, the coronavirus that causes the disease covid-19. The typical vaccine candidate takes years of research before it reaches clinical trials, while there are now at least three dozen covid-19 candidates that are in Phase I or further in the three-phase process.
Because there are so many vaccine candidates in development, using a variety of different approaches, it’s unlikely that we’ll fail to find at least one success story (typically, about 30 percent of vaccines that reach clinical trials are approved, according to a 2019 study). Still, President Trump set off astonishment and alarm among scientists and public health experts when he said recently that he expects a vaccine to be available by as early as late October, before Election Day.
Last week, Russia went one step further, announcing it has already approved a vaccine for use, codenamed Sputnik V. There is next to no information available about the Russian vaccine, including how effective it’s supposed to be or when it will actually be available to the public. On Wednesday, the country announced that it has started a Phase III trial of the already-approved vaccine, typically the last stage of clinical research needed before a drug or treatment wins regulatory approval from governments.
https://gizmodo.com/russia-approved-a-covid-19-vaccine-because-it-can-1844687352
Trouble is, there’s only so much you can safely speed up vaccine research. Roughly 30,000 people in the U.S. are expected to receive Moderna’s covid-19 vaccine in the Phase III trial launched in late July, one of the vaccine candidates furthest along. It will take months to dose every single person with the actual vaccine and to track whether they’re less likely to get covid-19 than a control group; then it’ll take more time to analyze that data in full, and more time after that for outside scientists to evaluate the data and make their recommendations to the Food and Drug Administration for approval or not. Other approaches, such as deliberately exposing a group of people to the virus, might sound quicker, but experts have said that it would still take up to a year to safely run such trials.
As much as everyone wants a vaccine to be out as soon as possible, few experts are willing to cut any of these steps to save time. One day after Steven Salzberg, a researcher and biostatistician at John Hopkins University, penned an op-ed in Forbes last week calling for a limited rollout of experimental vaccines to the public—one that received lots of criticism from fellow scientists—he penned another, titled I Was Wrong: We Can’t Skip Phase 3 Vaccine Trials.
It’s certainly possible the Trump administration could ignore all these experts (it’d hardly be the first time this has happened during the pandemic) and somehow rush a vaccine to the public just in time for Election Day. But even then, there would be major supply constraints that the world hasn’t come close to solving yet, let alone the personal dangers of taking a vaccine with no clear record of safety.
“Is it likely that there’s a vaccine in October? No, it’s not likely. Could it happen? Yeah, but I’m not sure I would take that particular vaccine,” said Julie Swann, a systems engineer at North Carolina State University who served as a science advisor on the U.S. vaccine rollout during the 2009 swine flu pandemic.
A more realistic if still very optimistic timeline could be the announcement of a successful candidate by the end of the year, with the rollout happening sometime in 2021. But again, that’s assuming everything goes according to plan.
How can we be confident it’s safe?
Anti-vaxxers aside, it’s understandable that anyone might have concerns about the safety of a vaccine developed in record time.
Right now, the safety signals we’ve been seeing from vaccine trials have been mostly encouraging, with no reports of severe side effects. At the same time, there have been relatively high rates of fever and other symptoms observed for some candidates. No vaccine or drug comes without side effects, but the benefits of any vaccine that sees the light of day should clearly outweigh the risks. While a highly effective vaccine that lowers the chance of infection by 90% or more would be ideal, the threshold of success establishedby the Food and Drug Administration is 50% effectiveness.
The fear that many experts and casual observers have is that a rushed process will throw away this basic guiding principle. And though the current head of the FDA, Stephen Hahn, has tried to reassure people that the FDA will only approve a safe and effective vaccine, the mixed messages from the Trump administration have understandably left people wary.
“I do not think a vaccine will be used without proper evaluation, but even the perception that an appropriate evaluation was not done could undermine not only vaccination against SARS-CoV-2 but confidence in all vaccines and seriously threaten public health,” said William Moss, an infectious disease and vaccine specialist at Johns Hopkins Bloomberg School of Public Health.
One way to assuage fears over safety is to make sure that people from all demographics are included in the clinical trials. People of color and pregnant women in particular have been historically excluded from clinical research. And it’s minority communities that have so far been disproportionately affected by the pandemic, both in their exposure to the virus and their risk of dying from it. The FDA, companies like Moderna, and researchers themselves have stated that they’re trying to ensure volunteer diversity in covid-19 vaccine research, but many early trials have still largely relied on the same homogenous populations that most trials recruit, and there’s no mandate that these trials have to be representative of the country’s population.
As Moss said, it’s the perception that matters greatly here. Rates of vaccine hesitancy have risen over the years, and while much of that hesitancy has been stoked by the false propaganda of the anti-vaccination movement, there are also legitimate issues of mistrust from minority communities toward the U.S. health care system, including when it comes to a covid-19 vaccine. Any successful mass vaccination campaign for covid-19 is going to have to overcome that hurdle.
Who will get it first?
There’s simply no way that we will have enough of any successful vaccine to go around, at least at first.
The U.S. government recently secured an agreement with Moderna as well as the pharmaceutical company Pfizer to manufacture and distribute an initial batch of 100 million doses each of their respective vaccine candidates. Though production is set to begin while clinical trials are ongoing, it’s expected that it will take until the end of the year to have all these doses ready, and in any case, that number is still less than one-third of the U.S. population. Both Pfizer and Moderna’s vaccine will also likely require a booster a month or more later, adding more strain on any available supply.
In light of the logistics, governments across the world and public health experts are already starting to hash out who should get the first doses of any vaccine. But any agreement that’s reached is likely to rankle.
“Several groups are thinking through what this prioritization process would look like at the state, national, and global levels, but no doubt it will be complicated and messy,” Moss said. “Most people agree that health care workers and those who are most vulnerable to severe disease, such as the elderly and those with other conditions, should be prioritized.”
During the 2009 H1N1 pandemic, Swann noted, there was an early controversy when it turned out that Wall Street employees hadjumped to the front of the line in securing the first scarce doses of the vaccine. Though we don’t know that something similar would happen with a covid-19 vaccine, we have already seen elite segments of society get preferential access to testing along with the resources needed to avoid exposure to the virus in the first place. If that same pattern repeats with vaccination, that too could seriously hamper people’s willingness to even take the vaccine.
“Eventually, perhaps a year after a vaccine is first available, there will be sufficient quantity for all who want to be vaccinated,” Moss said. “But not everyone wants to be vaccinated, in part because of disinformation and mistrust of science, authorities, and vaccines. A multi-pronged communication strategy is urgently needed to build the necessary trust so that those who are at greatest risk accept vaccination.”
How much will it cost?
This is probably the question with the most optimistic answer.
Both political parties were squirrelly early on in the pandemic about the potential out-of-pocket costs of a future vaccine. However, in mid-June, the White House announced that it expects insurers to cover vaccination without any copays involved; the administration also pledged that it would provide free vaccines to any “vulnerable” populations who could not afford it.
https://gizmodo.com/a-coronavirus-vaccine-should-be-free-not-affordable-1841976751
Legally, insurers have to cover all of the upfront costs of any vaccines that are recommended by the Centers for Disease Control and Prevention’s Advisory Committee on Immunization Practices—and it’s unlikely that any successful covid-19 vaccine wouldn’t meet that standard. But this is a mandate created by the Affordable Care Act, which the Trump administration has continued to try to destroy, even in the midst of the pandemic.
Will a vaccine bring back “normal” life?
The short answer is: No, not right away.
As discussed above, any successful vaccine will take time to be distributed to everyone who wants it, and in the absolute best-case scenario, that might be possible by the middle of next year. But there are so many unknowns between then and now.
The vaccines we’re seeing in Phase III trials now have all provoked an immune response in volunteers, but we don’t know how this response will translate to the real world in actually preventing infections, and experts have cautionedthat the first vaccines to see success may not be all that great. Even a mediocre vaccine would be immensely useful in preventing cases of serious illness and blunting the impact of future covid-19 outbreaks, but the dangers of the pandemic would still be present on some level.
In time, researchers may develop a vaccine that is highly effective, similar to many of the childhood shots now available for diseases like measles. But the example of measles also shows why we’re probably going to have to live with covid-19 for years to come, if not forever. Following decades of progress in slowly eradicating measles, the viral disease has started to make a comeback in Europeand the U.S., largely due to small communities of people unwilling to vaccinate their children.
It’s important to keep in mind that, despite vaccines having existed since the 1800s, humankind has only managed to eradicate one vaccine-preventable disease in people: smallpox. Hopefully, the novel coronavirus will someday be downgraded from a globe-shaking disaster to a mere nuisance of everyday life. But it’s doubtful that we’ll ever be rid of it completely. And the economic, social, and health repercussions of this pandemic are likely to reverberate long after the worst of covid-19 has passed.