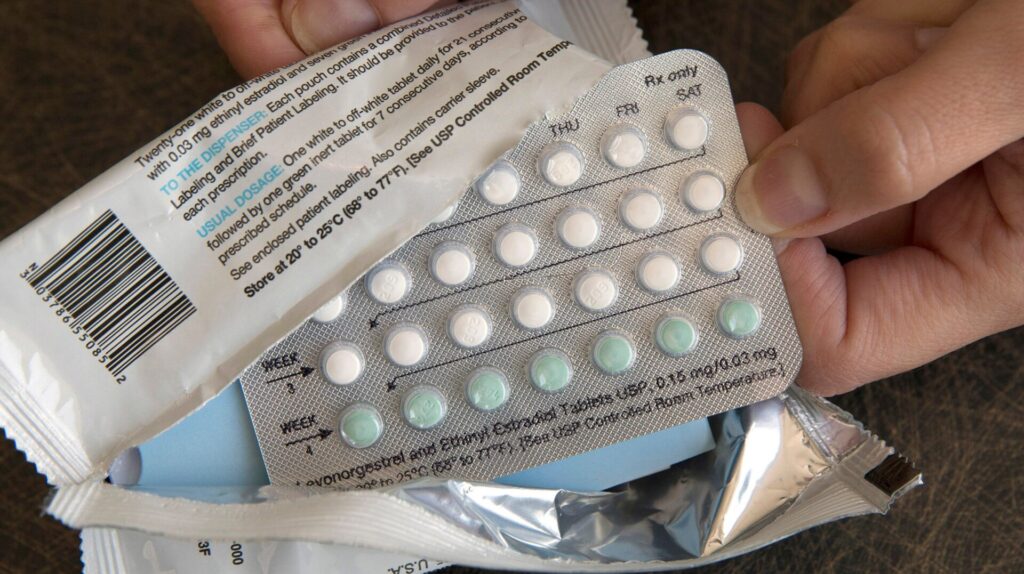
Teen birthrates are at an all-time low, but unintended pregnancies among young women are still a serious problem that disproportionately affects low-income families. A new study in The Lancet suggests that more training for healthcare providers could improve contraceptive use for these women.
Cynthia Harper, a professor at the Bixby Center for Reproductive Health at UC San Francisco, working with colleagues from Planned Parenthood and Columbia University, examined the effect of teaching healthcare providers at family planning and abortion clinics about current options for long acting reversible contraceptives (LARCs) like IUDs and progestin implants. Harper and her colleagues reasoned that if more healthcare providers knew about new types of LARCs, they could offer more choice to the at-risk women in their clinics.
Clinics in the study were randomly divided into two groups: half of the clinics got training specific to LARC use and insertion, the other half continued to recommend condoms and hormonal contraceptive methods. Women visiting the clinics were given the option to join the study; in total, 1500 women between the ages of 18 and 25 signed up, all of whom said they wanted to avoid getting pregnant.
Women joining the study were asked what type of contraception they had used over the previous three months. The following chart visualizes their responses:
These results aren’t really surprising: Most young women in the United States don’t use LARCs, because in the US, LARCs are usually first offered to married women, after they’ve had children. They also show that even when young women are using hormonal or barrier methods, they may sometimes have unprotected sex.
After their initial appointment, the women were surveyed to find out what types of contraceptive they’d learned about at the clinic, and whether or not they’d decided to try a LARC.
The study found that if clinicians are trained in the use of LARCs, they’re more likely to tell their patients that the option exists. If young women know about LARCs, they’re more likely to use them to prevent pregnancy.
But the study also found that when it came to reducing pregnancy rates, the place that women received contraceptive counseling mattered. Women who visited family planning clinics had fewer pregnancies over the course of the study than the women who had been recruited at abortion clinics.
The researchers believe this difference is due to the higher cost of contraceptive methods like IUDs (38% of study participants reported they had no insurance), combined with the extra steps required to get the devices.
…although women chose LARCs after abortion, fewer were able to obtain them than women attending family planning visits (44% vs 73%). Cost barriers to uptake of contraception are high in the abortion care setting in the USA… In some states, women must return to a family planning clinic to qualify for contraceptive coverage. Increased pregnancy risks are associated with an increased number of visits, and an estimated 30% of women do not return after abortion for IUD insertions.
[Source: Finer et al. 2012 | Harper et al. 2015]
Contact the author at [email protected]. Top image Ceridwen~commonswiki via Wikimedia | CC-BY-SA 2.0 fr. All charts by the author.