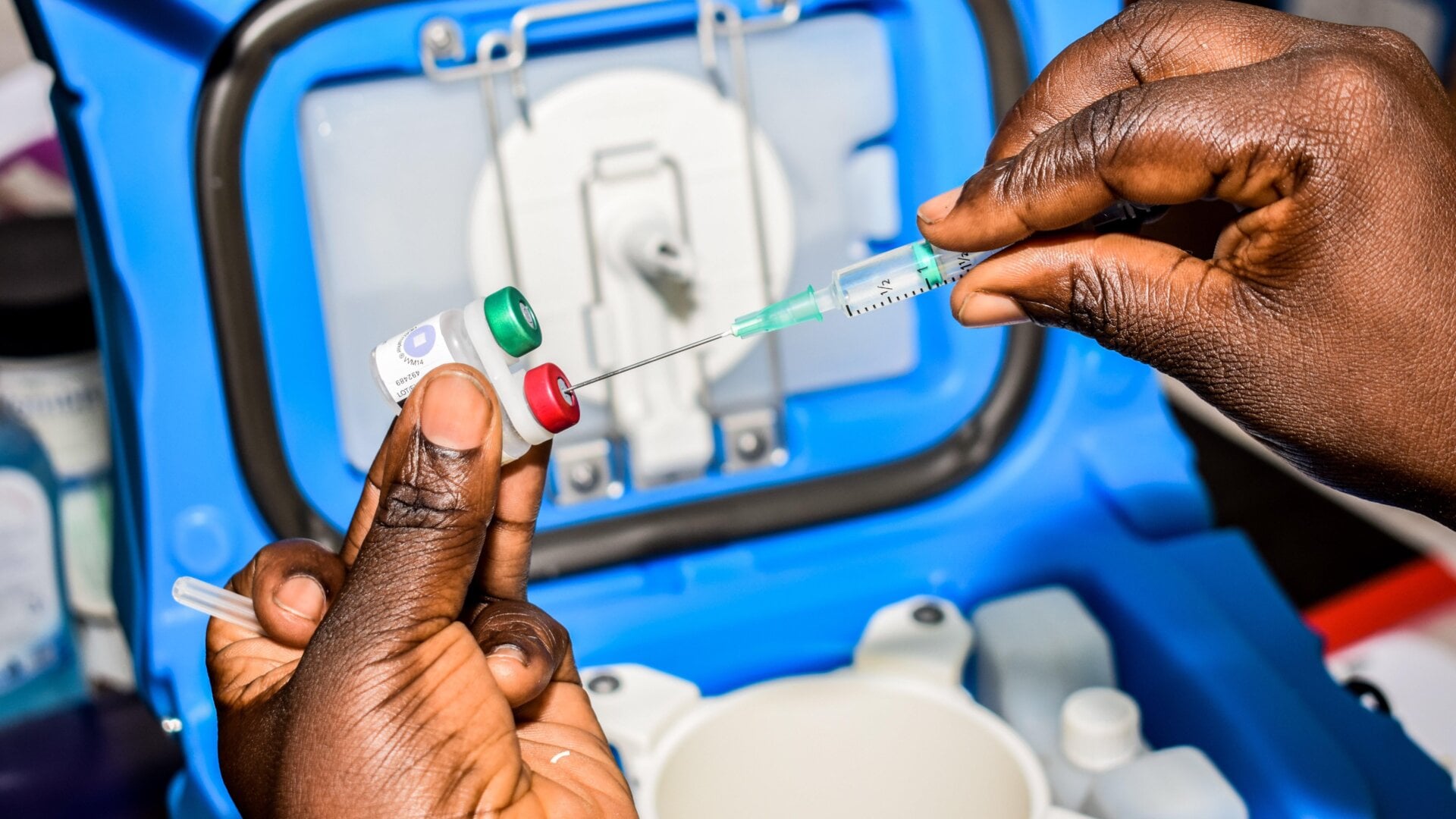
The fight against malaria, one of the world’s worst diseases for decades, is likely to get much easier as the World Health Organization has endorsed the wide use of a malaria vaccine developed by GlaxoSmithKline, the first ever to win such approval. The vaccine will be recommended for children in sub-Saharan Africa and other high-risk areas as a four-dose schedule starting at age 5 months.
Malaria is a mosquitoborne infection caused by at least five species of the Plasmodium parasite. Most infections are from Plasmodium falciparum and Plasmodium vivax, with the former causing most cases in Africa. Early symptoms of malaria tend to be mild and include fever, headache, and chills, but P. falciparum malaria can lead to severe organ damage and death if left untreated, especially in younger children.
Malaria cases and deaths have declined in recent decades, thanks to dedicated mosquito control and treatment programs. But there were still 229 million cases estimated worldwide in 2019, along with around 400,000 deaths—a toll second only to tuberculosis for a single infectious disease (covid-19 has since overtaken malaria and likely TB in the past two years). Precarious progress against malaria has been threatened further by the emergence of insecticide resistance among female Anopheles mosquitoes, the vectors of the disease.
The continued threat of malaria has made the prospect of a childhood vaccine all the more tantalizing. But developing a vaccine against a complex organism like a parasite has proven to be much more difficult than it has been for simpler bacteria and viruses, and for decades, scientists have come up short. Until now, it seems.
“This is a historic moment. The long-awaited malaria vaccine for children is a breakthrough for science, child health and malaria control,” said WHO Director-General Tedros Adhanom Ghebreyesus in a statement announcing their endorsement of the vaccine. “Using this vaccine on top of existing tools to prevent malaria could save tens of thousands of young lives each year.”
Despite the good news, GlaxoSmithKline’s vaccine, which is currently code-named RTS,S/AS01 but will be branded as Mosquirix, is only modestly effective. In the clinical trials evaluated for WHO approval, it was found to prevent around half of severe cases caused by P. falciparum malaria, compared to the control group. But this level of efficacy was only seen in the first year of vaccination, and by the fourth year, protection had waned to very low levels. At roughly 55% efficacy, the vaccine meets the bare minimum for WHO endorsement.
A major study this year did find that a combination of the vaccine and anti-malarial drugs can further reduce the risk of severe disease and death by 70%, a much more appealing target for public health programs. But even as is, one study has projected that the vaccine would prevent millions of cases and over 20,000 deaths annually in sub-Saharan Africa if deployed widely.
Like other vaccines before it, Mosquirix may also represent the first step toward more effective vaccines in the future. There are several other candidates in development already, including one from Moderna that’s relying on the same mRNA platform as the company’s successful covid-19 vaccine.