An aesthetically unpleasant but genuinely promising medical treatment—a fecal transplant—may come with more serious risks than previously thought. This week, the Food and Drug Administration issued a warning about the treatment, after receiving reports of two people coming down with serious drug-resistant infections following the procedure. One patient ultimately died.
Fecal transplants, or fecal microbiota transplantation (FMT), have been explored as a way to reset the delicate bacterial environment of a person’s gut. A recipient’s gut microbiome is scrubbed out as much as possible with heavy-duty antibiotics, then the donor’s gut bacteria is transplanted over, which will hopefully seed the gut with a healthy balance of bacteria again. Most FMTs are performed via an enema, though doctors are studying if a capsule of the donor’s gut bacteria taken orally can work just as well.
A gut microbiome imbalance is thought to contribute to conditions like irritable bowel syndrome, inflammatory bowel disease (IBD), and possibly even metabolic diseases like obesity. So far, though, the clearest potential for FMT has been for people with a recurrent, often excruciating infection of Clostridium difficile, or C. diff. Cure rates of recurrent C. diff with FMT have hovered as high as 90 percent in small trials.
https://gizmodo.com/why-does-coffee-make-us-poop-scientists-gave-coffee-to-1834852779
FMT at this point is an experimental treatment, however. And trials are still ongoing that are trying to figure out how to make the procedure as effective and safe as possible. According to the FDA, the two superbug infections were spotted in such a trial.
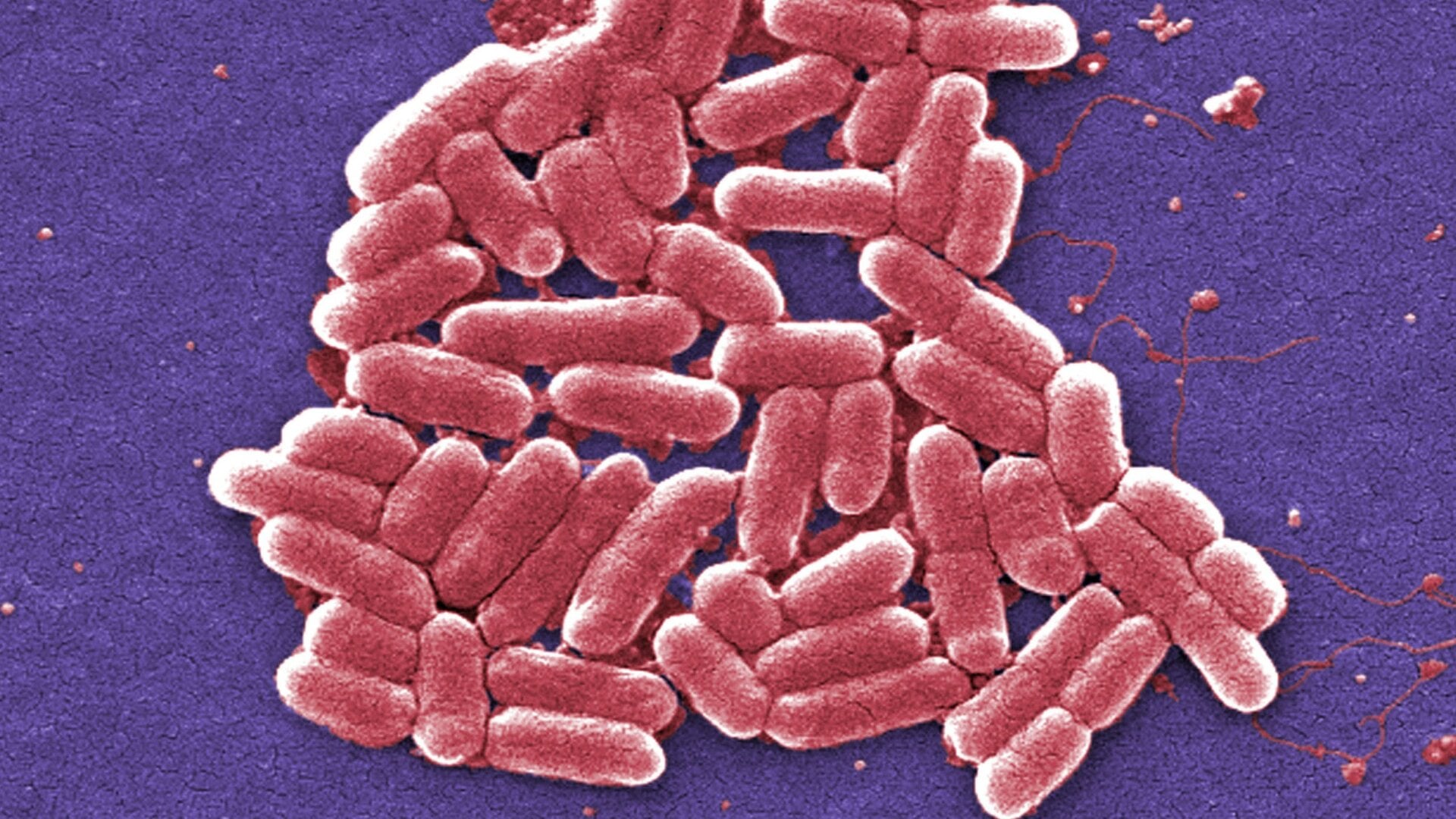
The patients were part of an investigational FMT trial, and received a transplant from the same donor. Soon after, they developed an invasive infection caused by multidrug-resistant Escherichia coli (E.coli). Despite doctors’ efforts, one patient didn’t make it through. In the aftermath, the donor’s remaining samples were tested and the same E. coli strain was discovered.
“FDA is informing members of the medical and scientific communities and other interested persons of the potential risk of transmission of [multidrug-resistant organisms] by FMT and the resultant serious adverse reactions that may occur,” the agency said in its safety communication.
It’s likely that the pre-existing health of both patients contributed to the severity of their illnesses, since both had weakened immune systems. But the infections could have been prevented had doctors in the trial been looking for these bacteria in donors to begin with, the FDA said.
In 2013, as FMT trials began taking off, the agency announced it would take a hands-off approach in regulating its early use for C. diff infections (generally, any new drug or treatment for a disease needs to go through a lengthy FDA approval process before it can be widely available). So long as patients were told upfront about the potential risks and experimental nature of the treatment by doctors, it would be less strict in approving or supervising new clinical trials. But as a result of these tragic cases, the agency is now demanding that all investigational trials preemptively screen their donors for risk factors that would make them more likely to have superbugs, as well as to test their donor samples for these bacteria. Doctors should tell their volunteers beforehand about these now-discovered serious risks, too.
“Today’s safety communication underscores the importance of why new therapies are thoroughly studied to ensure the benefits of taking them outweigh the risks to patients, and we will continue to aggressively monitor clinical trials to ensure patients are protected when safety concerns arise,” Peter Marks, director of FDA’s Center for Biologics Evaluation and Research, said in an FDA statement.