In 1985, a premature baby was born in Maryland who needed surgery to tie off a dangerous blood vessel near his heart. The newborn, Jeffrey, died weeks after the procedure. His family learned afterwards that none of the procedures had been performed with analgesics; the only drug administered was a muscle relaxant.
The press ran with the story, alerting Americans to the grim realization that hospitals in the United States routinely operated on critically ill premature babies without giving them painkillers. “Most adults would be shocked if they saw what was done to children in hospitals without anesthetics,” said Myron Yaster of Johns Hopkins in a subsequent Baltimore Sun article. “It’s like roping and holding down a steer to brand it.” Jeffrey’s parents took action, leading to the 1987 declaration by the American Academy of Pediatrics that it was no longer ethical to perform surgery on preterm babies without anesthetics.
It’s been nearly 30 years since the AAP declaration, but to this day, many procedures are performed on newborns without the benefit of analgesics. That’s largely because of an enduring misconception in the medical community that newborns don’t feel pain like adults.
Two years ago, a review of neonatal pain management in intensive care units (NICUs) in Europe found that newborn babies experience 11 painful procedures each day on average, but that 60 percent of these babies weren’t receiving any kind of pain relief. That’s in keeping with common practice in the United States and Britain, where less than 35 percent of infants undergoing painful procedures received any kind of analgesic to manage their pain. These procedures ranged in scope from the very mild, such as taking blood samples, to more invasive interventions, like chest tube insertions and circumcisions.
https://gizmodo.com/how-drugs-work-to-help-you-ease-the-pain-1452216695
And the latest scientific evidence shows unequivocally that newborns not only experience pain, but that they experience it more intensely than adults. The medical community is proving slow to respond. And experts who speak out continue to face ridicule and censure.
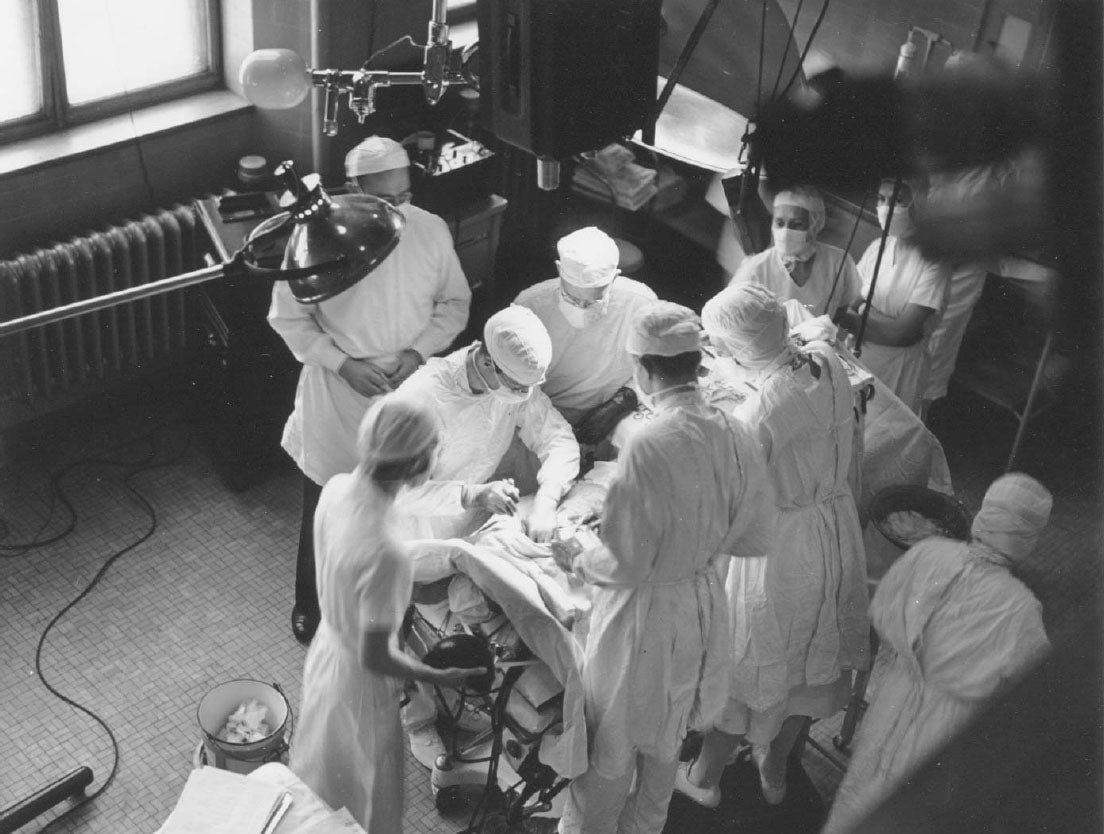 Groundbreaking cardiac surgery for newborns in 1945 at Johns Hopkins. A nurse can be seen at the head of the table administering anesthesia. Via The Alan Mason Chesney Medical Archives of The Johns Hopkins Medical Institutions.
Groundbreaking cardiac surgery for newborns in 1945 at Johns Hopkins. A nurse can be seen at the head of the table administering anesthesia. Via The Alan Mason Chesney Medical Archives of The Johns Hopkins Medical Institutions.
Prior to the Second World War, surgeries performed on babies were often fatal. Physicians began to administer anethesia to infants in the 1940s and 1950s, but many infants experienced cardiac arrest and brain damage. Their tiny bodies couldn’t sustain the metabolic and circulatory effects of these potent anesthetics. Discouraged, surgeons started to wonder if anesthesia for infants was even necessary.
It was also around this time that clinical psychologist Myrtle McGraw began to study the reactions of newborn infants to various stimuli, including pinpricks. Her experiments, conducted at Babies Hospital in New York City, showed that babies who had been fed and swaddled did not react to pinpricks, and that those who were awake did not have a specific response to pinpricks on parts of the body that were stimulated. In her subsequent research paper, McGraw assumed that the infants’ more generalized startle response was not a specific response to pain, and concluded that babies don’t perceive pain—at least not in the way that adults do. Her research was integrated into medical textbooks and became standard.
Over the next three decades, it was common to perform surgery on newborn infants using no anesthetics or pain relief. To prevent babies from squirming and thrashing around, surgeons administered neuromuscular blocks (muscle relaxants). Doctors essentially paralyzed their patients for surgery.
“What many people failed to acknowledge in the years following McGraw’s work was that pinpricks are a minor injury, or that they may not even cause any tissue injury at all,” said Kanwaljeet J. S. Anand, professor of Pediatrics and Anesthesiology at the Stanford University School of Medicine, and a pioneer in the study of infant pain. “Surgical operations, on the other hand, they’re a lot more invasive.”
The situation started to change in the late 1970s and early 1980s, culminating in the AAP decision. But the idea that babies don’t really feel pain persisted, and doctors continued to be wary of using painkillers on babies. “Neonatal circumcision is one common surgical procedure,” Anand said. “The use of analgesia or sedation or local anesthetic is not widely prevalent for this.” Other procedures routinely performed on infants include immunizations, blood extractions, and the placement of IV catheters and chest tubes, usually without analgesia.
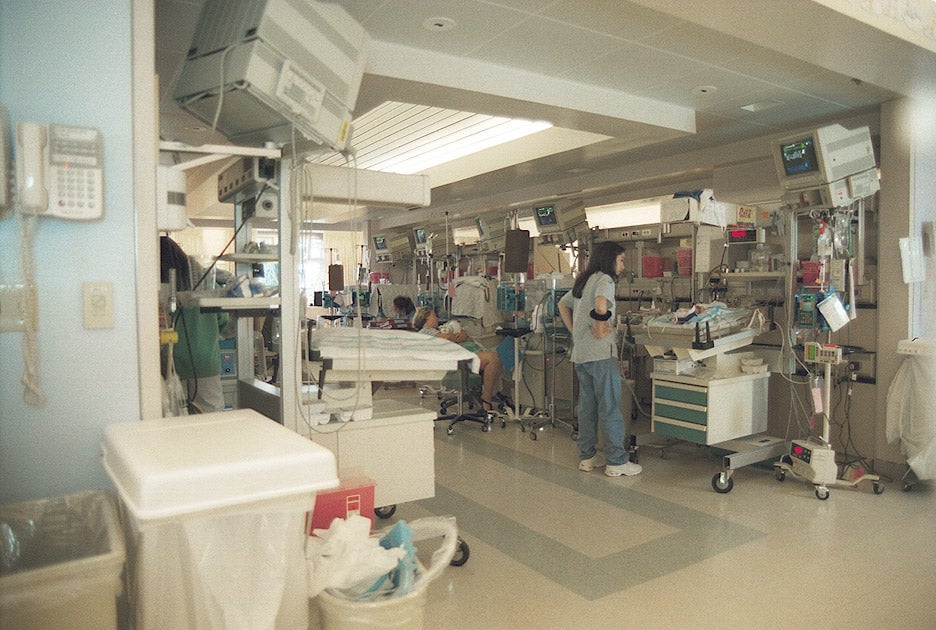 A neonatal intensive care unit in Hawaii. Via Kapi’olani Medical Center
A neonatal intensive care unit in Hawaii. Via Kapi’olani Medical Center
To get a sense of what routinely occurs in hospitals today, we talked to a bedside nurse who works at a NICU and asked to remain nameless. She requested anonymity for fear of losing her job; her opinions on infant pain are not shared by many of the doctors she works with.
“I’ve heard doctors say that they don’t believe babies—especially premature babies—feel pain the same way as adults because their nervous system (and/or musculoskeletal system) is not fully developed,” she explained to Gizmodo in an email. “Clinically this does not seem to be the case.”
Recently, her unit had an infant patient whose brain stopped developing late in the first trimester. Fluid had accumulated in the baby’s ventricles, putting pressure on her brain. Yet the doctors didn’t think she could be in pain because her brain was so underdeveloped. The nurse also cited instances of doctors skipping pain medication for children who have chest tubes, are intubated, or are uncomfortable because they have an accumulation of excess fluid.
“Chest tubes are very painful,” she said. “Endotracheal tubes are uncomfortable—just imagine a rigid rubber tube shoved down your throat trying to breathe for you. Our ventilators are quite smart and try to breathe with the child as much as possible so that they are not fighting the vent. This doesn’t always work. Babies will be sedated if they are fighting the vent so much that we cannot properly ventilate them.”
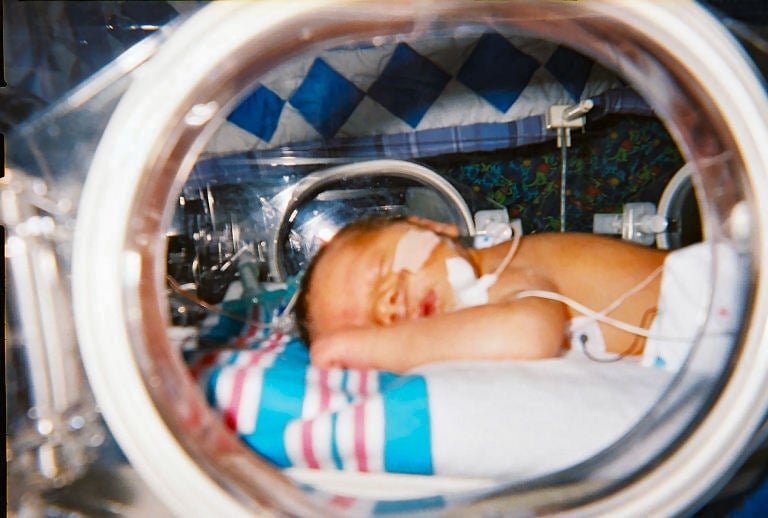 A newborn sleeping in an incubator. Via Zerbey CC BY-SA 3.0.
A newborn sleeping in an incubator. Via Zerbey CC BY-SA 3.0.
The doctors in her unit don’t administer pain relief for gastroschisis, a condition whereby an infant is born with their bowels, and sometimes other organs, on the outside. To treat it, a medical team will put the bowels and organs in a pouch and hang it above the infant, so the pouch can slowly descend into the abdominal cavity. But because the organs develop outside of the body, they must be put back in slowly so that the cavity has time to expand. Sometimes, surgeons will assist the process by slowly pushing a little intestine inside.
“We like to give pain medication for this procedure and our neonatologists are usually pretty good at ordering this, but the surgeons don’t like it,” the nurse said. “They are of the opinion that the procedure doesn’t hurt because the intestines do not have pain receptors. However, the skin that has to stretch to accommodate these organs do have pain receptors—and just imagine if someone put a heavy weight on your stomach, it wouldn’t be pleasant. Our patients do not tend to tolerate the procedure very well without pain medication. Their PIPP scores are often quite high.”
PIPP refers to the Premature Infant Pain Profile (pdf), a behavioral measure of pain for premature infants. Other similar scales exist, including the Neonatal Infant Pain Scale (NIPS), Pain Assessment in Neonates (PAIN), the Neonatal Assessment of Pain Inventory (NAPI), and many others. But there’s a surprising lack of standardization between them.
https://gizmodo.com/why-do-we-experience-physical-pain-5946522
Indicators on the PIPP profile include gestational age, changes to behavioral state, heart rate, oxygen saturation, and physical indicators such as nostril flaring, bulging brows, and eye squeezing. But even armed with the PIPP, nurses have trouble translating behavioral cues to pain.
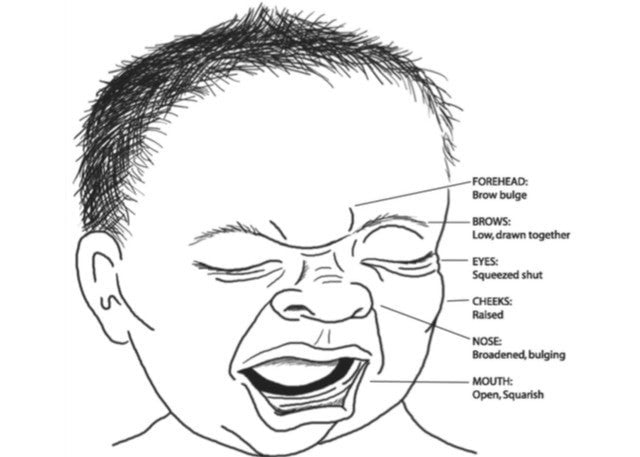 PIPP illustration. Via Royal Hospital for Women.
PIPP illustration. Via Royal Hospital for Women.
“Most normal baby behaviors are reflexive, including feeding,” said the nurse. “Reflexes are so primitive that it is difficult to assess the cognitive status of these children. If we can’t even discern cognitive status in these infants, how can we be expected to appropriately assess something as subjective as pain?”
Anand said he wasn’t surprised by the nurse’s experiences. “I think these surgeons are not well informed about the nature of pain,” he said. Preterm babies in particular are at risk, as they’re the ones most likely to be exposed to the greatest number of painful stimuli in the NICU. They also happen to be the smallest and sickest.
Since babies can’t talk, behavioral measures of pain are important, even if they’re limited and open to interpretation. Pain can be judged by looking at changes to physiology, and later by looking at changes in psychology, such as an aversion to certain stimuli.
But neurological evidence is emerging as well. A pioneering study conducted at Oxford University last year, led by Rebeccah Slater, used fMRI to scan the brains of 10 healthy infants aged one to six days old, and 10 healthy adults aged 23 to 36. The researchers poked subjects’ feet with a special device that retracts upon contact. “It’s a bit like poking the baby with a blunt pencil,”said study co-author and Oxford postdoctoral researcher Caroline Hartley.
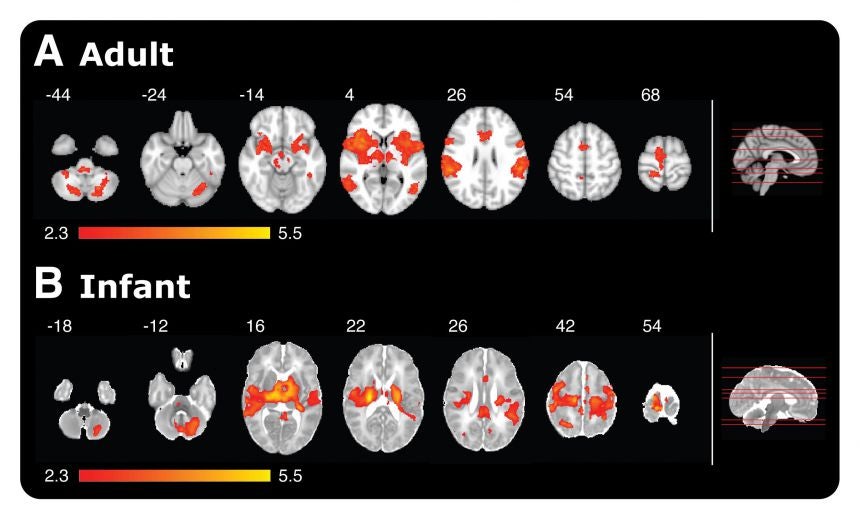 Brain scans showing activity in adults and babies when poked with a special retracting rod. Red-yellow colored areas show active brain regions. Via University of Oxford.
Brain scans showing activity in adults and babies when poked with a special retracting rod. Red-yellow colored areas show active brain regions. Via University of Oxford.
The team found that babies respond in a very similar way to adults. In fact, 18 out of the 20 brain regions activated in adults were also activated in babies, including brain regions that tell us where a given stimulus is on the body, and those that tell us a stimulus is unpleasant. The brains of the newborns exhibited the same response to a weak stimulus as the adults did to a stimulus four times as strong, suggesting that babies might be more sensitive to pain that adults.
Scientists at the Goldsmiths InfantLab at the University of London have shown that babies feel tickles differently from adults. This study, published in Current Biology, describes the phenomenon as “tactile solipsim,” a developmental stage in which babies are incapable of relating touch to an object or event outside of themselves. As lead author Andrew Bremner explained in Brain Decoder, “They just feel the touch as a touch on their body and that’s all. To me this idea of what it would be like to be a baby feeling a touch is quite strikingly different to our own realities.”
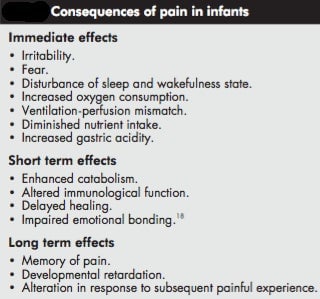 There are consequences to ignoring infant pain. A 2003 study published in the British Medical Journal listed several, including immediate effects like irritability, fear, and sleep disturbance, short term effects such as a diminished immune system, and long term effects like ongoing memory of the pain and even developmental delays. Study after study has shown that babies who are given pain relief consistently exhibit better medical outcomes.
There are consequences to ignoring infant pain. A 2003 study published in the British Medical Journal listed several, including immediate effects like irritability, fear, and sleep disturbance, short term effects such as a diminished immune system, and long term effects like ongoing memory of the pain and even developmental delays. Study after study has shown that babies who are given pain relief consistently exhibit better medical outcomes.
So why the reluctance? There are multiple factors at play. According to Anand, there’s “a somewhat extravagant concern” about the side-effects or toxicities of pain relieving agents in newborns. He said there is still a “diehard notion” among some practitioners that babies should not be given painkillers.
Analgesic drugs do have side-effects, and if used indiscriminately they can cause severe problems for babies. Exposure in the absence of pain will change a baby’s brain development, and can cause a newborn to develop a dependence on the drugs.
“So herein lies the rub,” said Anand. “We have to use our clinical acumen to judge the degree of pain that is being produced by a particular procedure, and use analgesia in a judicious way to take away that degree of pain, or at least lessen the intensity of that pain. I’m all for the judicious use of analgesia and for avoiding large or prolonged doses of drugs.”
Changing medical culture around the treatment of newborns won’t happen overnight, but it’s not an intractable problem. Pain management should be incorporated into medical training, and workshops and online resources should be made available. A recent study done in Europe found that countries with nationally accepted guidelines, such as Sweden, the Netherlands, and France, did much better in treating neonatal pain than those without. The US and Canada are lagging behind. In 2001, an international consensus group on neonatal pain tried to get the ball rolling on the development of standardized national guidelines, but not much has been done since then.
When Anand began his work in the 1980s, he found that people were eager to deny and denigrate the information he was presenting.
It was as if the medical community as a whole was experiencing cognitive dissonance on the matter, afraid of having to confront the truth and go to the trouble of overturning standard medical convention.
“My career has taken a hit because of my commitment to getting people to pay attention to this aspect of newborn care,” Anand said. “Grant funding has also been very difficult. Obviously, I’m committed to the babies whose suffering needs to be acknowledged.”
[ Sources: Sezgi Goksan et al., 2015: “fMRI reveals neural activity overlap between adult and infant pain” | K. J. Anand et al., 1987: “Pain and its effects in the human neonate and fetus” | D. W. Roofthooft et al., 2014: “Eight years later, are we still hurting newborn infants?” | Goldsmiths InfantLab 1, 2 | P. Matthew et al., 2003: “Assessment and management of pain in infants” | American Academy of Pediatrics ]
Top image: Jim Cooke