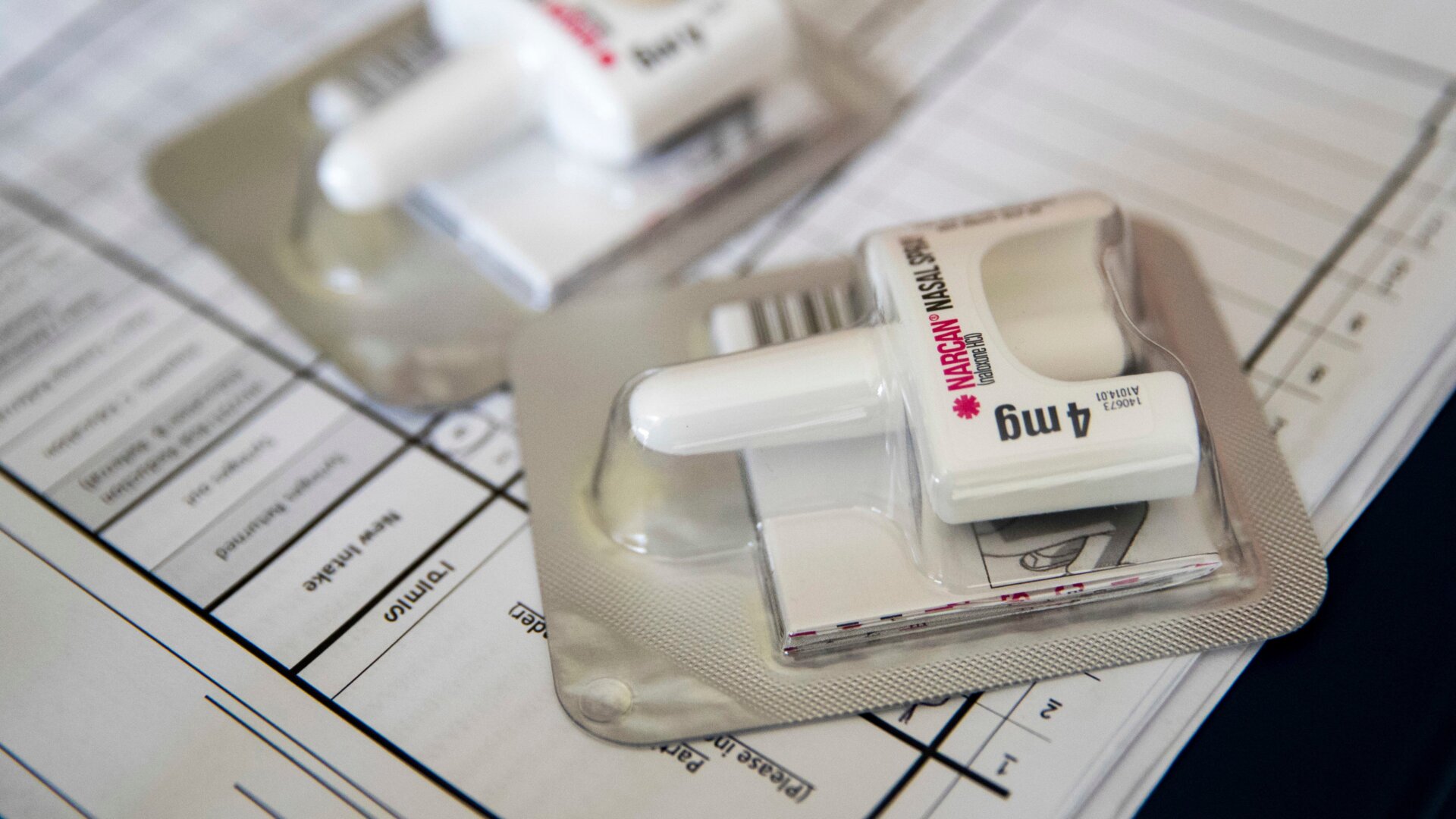
There have been few glimmers of hope when it comes to the opioid crisis. But a new report this week from the Centers for Disease Control and Prevention suggests that many more people are now getting access to the opioid overdose antidote naloxone—and that may have helped slightly reduce the number of opioid-related deaths in 2018. At the same time, there are still areas of the country that aren’t getting the naloxone they need.
The report, published as part of the CDC’s regular Vital Signs series, looked at the number of naloxone prescriptions that were dispensed from store pharmacies over a seven-year period. The CDC relied on a database that accounts for 92 percent of all retail prescriptions dispensed on a county level. Between 2012 to 2018, they found, naloxone prescriptions dramatically rose. In 2012, there were only 1,282 such prescriptions. But in 2018, there were 556,847 naloxone prescriptions, slightly more than double the prescriptions made in 2017.
Prescription opioids are no longer the most common type of opioid involved in overdose deaths, with synthetic opioids like fentanyl now ranking highest. Nor do most people who take prescribed opioids develop a substance-use disorder or suffer an overdose. But in 2017, prescribed opioids were still involved in around 17,000 fatal overdoses (often, more than one drug is involved in an overdose, and not all people who have died from prescribed opioids legally obtain them).
Because the risk of overdose can increase when people are given high-dose opioid prescriptions, the CDC has recommended since 2016 that doctors should also prescribe naloxone to these patients. Some states have legally mandated the same for their doctors. So the substantially higher amount of naloxone prescriptions (and fewer high-dose opioid prescriptions) last year might have prevented some deaths.
https://gizmodo.com/opioid-maker-purdue-promises-not-to-profit-from-its-new-1833334488
According to a preliminary report by the CDC released last month, the number of total overdose deaths may have actually declined in 2018 by 5 percent, from the record high of 72,000 deaths in 2017. Opioid-related overdoses also likely took a slight decline, from around 49,000 deaths in 2017 to a projected 47,600 in 2018.
But the CDC authors noted there’s still much more that should be done. Only one in every 69 high-dose opioid prescriptions in 2018 came with naloxone, they found. And while half a million naloxone prescriptions isn’t nothing, there would have been almost 9 million prescriptions that year if every doctor had followed the CDC guidelines. Areas of the country with high rates of opioid prescribing and overdose deaths as well as greater access to substance-use treatments like buprenorphine were also more likely to prescribe naloxone. But rural regions, which have been disproportionately affected by overdose deaths, were less likely to have high rates of naloxone prescribing than cities.
Naloxone prescriptions aren’t the only way to ensure that people can be saved when they have an overdose. Some states have passed laws that allow pharmacists to dispense naloxone to people without a prescription, and public health experts have long called for the government to approve an over-the-counter naloxone product. In January, the Food and Drug Administration announced it would streamline the process for companies to develop and bring to market OTC naloxone, while a generic nasal spray version of the drug was approved this April.
In the meantime, the authors wrote, there are still ways to improve people’s access to prescription naloxone. That includes lowering the out-of-pocket costs for Medicare patients, since they often have higher co-pays than those on private insurance; educating doctors and patients about the value of naloxone; and creating or further funding programs that distribute naloxone to people living in high-risk and rural areas.
“Distribution of naloxone is a critical component of the public health response to the opioid overdose epidemic,” the authors wrote.