The official tally of covid-19 in America is climbing steeply as more people are finally being tested, with at least 80,000 people tested and more than 8,000 reported cases as of March 19. But preliminary forecasts created by epidemiologists paint a far grimmer picture of the novel coronavirus’s spread in the U.S.: We may already have tens of thousands of cases and possibly more than 150,000.
The first known cases of covid-19, caused by the coronavirus SARS-CoV-2, were reported by the Chinese government late last December (though cases were likely occurring at least as far as back as November). By January 21, the first known imported case was documented in the U.S.; a month later, the first known local case was documented in California. But as even covid-19 has spread to more than 110 countries and all 50 U.S. states, we still know shockingly little about how prevalent the disease is in the U.S., thanks to a minuscule supply of test kits available up until very recently. One study found that the virus may have been circulating undetected among people in Washington state as early as mid-January.
This week, researcher Alex Perkins, an infectious disease epidemiologist at the University of Notre Dame, and his team released a paper on the preprint server Medrxiv. Using data from local and imported cases in the U.S., along with knowledge gleaned from the outbreaks in China and Singapore, they tried to predict how many undocumented and total covid-19 cases were likely here on March 12, the day before President Donald Trump declared a national emergency over the outbreak.
By their estimation, there were likely 22,876 actual cases as of March 12. Their range of predictions, though, went from a low of just over 7,000 cases to a high of over 53,000 on March 12. According to Perkins, there are several factors crucial to how low or high the estimates were.
“Two in particular that are important are the reproduction number, R, which is how many people you go on to infect once you’re infected, and the generation interval, which is how long it takes for you to infect those people after you get infected,” Perkins told Gizmodo. “The reason those factors are so important is because they determine how many people could have gotten infected within a given timeframe.”
Perkins’ team isn’t the only one trying to predict covid-19’s path through the U.S. A pair of researchers at the University of Massachusetts Amherst, Andrew Lover and Thomas McAndrew, recently released their own paper. They used a different method of forecasting. It largely relied on “sentinel events,” or individual instances where covid-19 did or could have spread far, to inform the team’s assumptions. These sentinel events include both the Wuhan outbreak in China and the Conservative Political Action Conference in Maryland in late February, where at least one person came down with covid-19 and may have infected others.
“Looking at the CPAC conference, there are about 20,000 participants. And there was a pretty good nationwide selection of people as far as we can tell. So there are people from every state in probably all age groups,” Lover told Gizmodo. “So using the one case that was confirmed out of the 20,000, we then extrapolate that to the full U.S. population of 329 million. And we can estimate about how many new cases there were on March 1.”
From there, they projected out to March 12, as Perkins’ team did. Their basic conclusion was remarkably close to Perkins’ bleaker forecast, with a median 54,000 cases estimated as of March 12. Their high-end estimate went as high as 125,300 cases by that date.
Fellow UMass researcher Nicholas Reich, a biostatistician, decided to collect and analyze the estimates of Perkins, Lover, and others (including a poll conducted of experts by Reich) to graph out the likely trajectory of cases up to March 17. The graph, credited to Reich, Lover, and McAndrew, was shared with Gizmodo. The blue line indicates the most likely route of covid-19 cases up until March 17 under Lover and McAndrew’s original model, while the grey represents the uppermost projection of their model, within an 80 percent certainty.
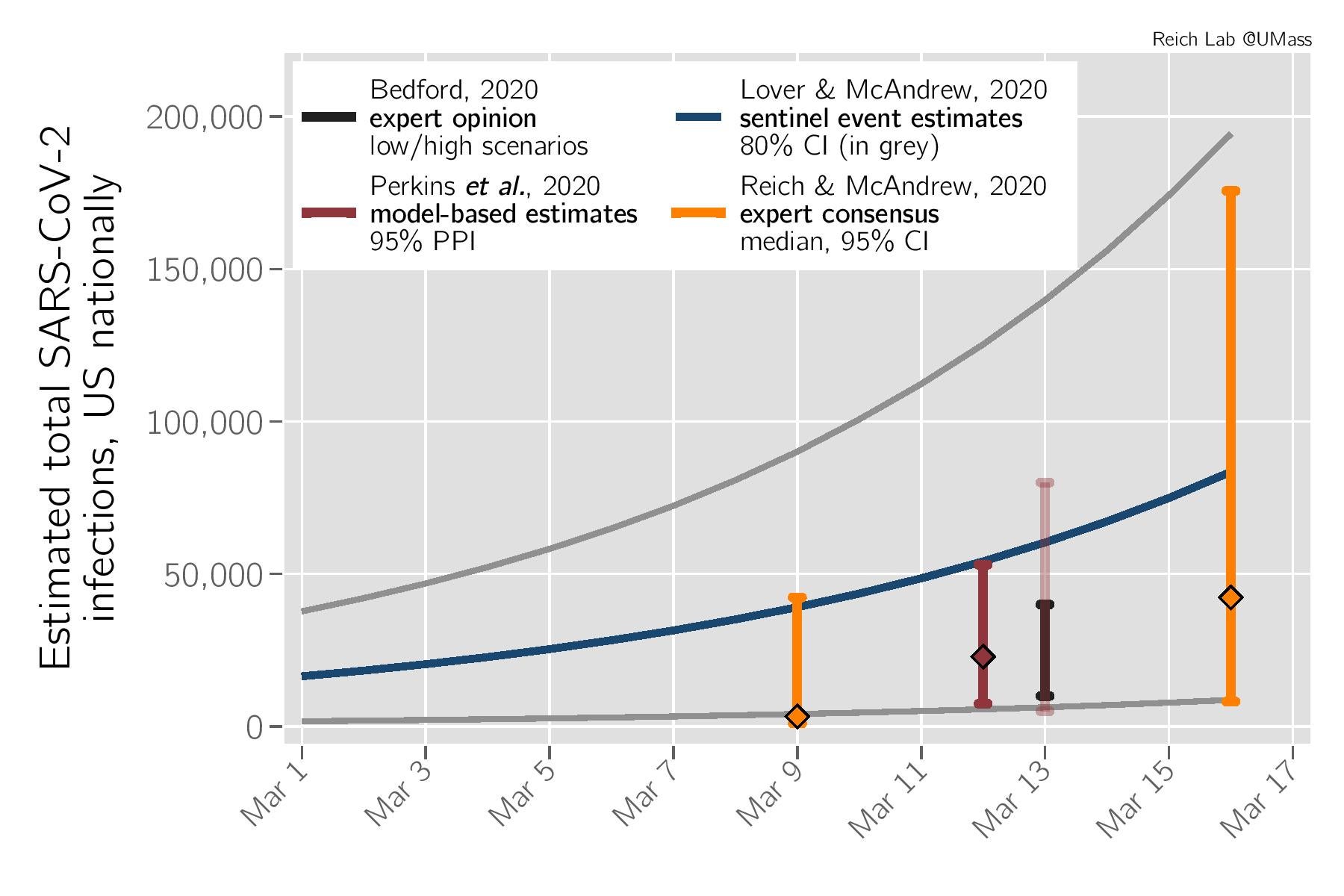
“We have all been struck at how consistent these estimates are, despite being from different research groups each using quite different techniques,” Reich told Gizmodo. “The bottom line is that the reported cases that we see from CDC and state health departments really are capturing just a small fraction of the total number of total infections from SARS-CoV-2.”
To be clear, these estimates are preliminary and haven’t gone through the typical peer-review process. Even if accurate, they may not tell us much about how bad things will get.
“Forecasting any infectious disease more than a week or 10 days is pretty, pretty challenging. And especially in this case, we don’t know that much about the transmission,” Lover said. Even with data from China or elsewhere, it’s still possible that covid-19 hasn’t or won’t spread at the same rate here as it did in other places.
It’s true that the U.S. has only recently started to enact or contemplate the sort of drastic actions to reduce transmission that countries such as South Korea—touted for its fast, so far effective response to covid-19—have. But that’s not to say that these actions can’t have a real impact on the course of the disease from this point on.
Some researchers have argued that if U.S. testing capability improves greatly, to the point where we can quickly find and isolate potential clusters as South Korea has done, we can still substantially drive down cases and deaths in the months to come. We might be able to do this without necessarily having to keep ourselves completely isolated from one another for the next 18 months. While some experimental treatments for covid-19 haven’t panned out in small trials, others seem promising. Any effective treatment could obviously cut down the huge number of deaths predicted.
But even without these hopeful developments, we can do something right now to stem covid-19, as Perkins notes.
“We’re well on our way to this being a bad situation, but there is a lot we can do to prevent it from being even worse. Social distancing is key to achieving that, as is continued testing and isolation,” he said. “As people see the numbers of cases and deaths continue to rise for a while, they need to keep in mind that those numbers would have been even worse if we weren’t taking the measures that we are.”






