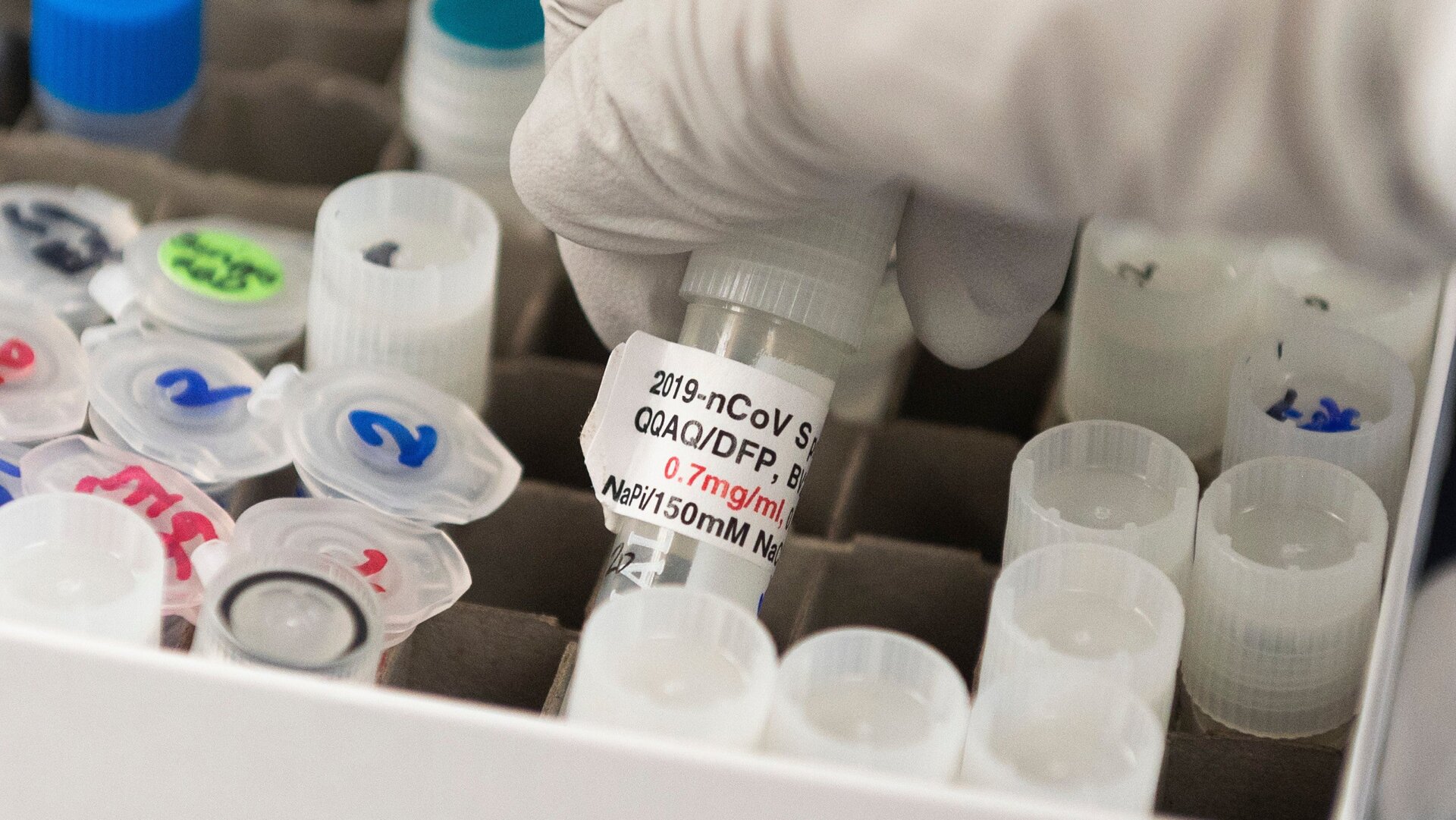
The end of the week has brought along a flurry of encouraging news on the second wave of covid-19 vaccines being tested in trials around the world.
Recent clinical trial results from the companies Johnson & Johnson and Novavax suggest that both their experimental vaccines are highly effective at preventing serious illness and hospitalization, while being well-tolerated. Yet, the findings also suggest they’re less effective against a variant of the coronavirus that’s become widespread in South Africa and is spreading elsewhere. Meanwhile, another vaccine—Oxford University and AstraZeneca’s candidate—was just granted emergency use approval in the European Union.
On Thursday, Novavax announced results from its trials in the UK and South Africa. The Phase III trial results in the UK indicate that the candidate is around 89% effective at preventing symptoms from coronavirus infection. Importantly, the trial took place during a time when a new variant in the country—dubbed B.1.1.7—was just starting to circulate widely. Despite B.1.1.7 being noticeably more transmissible and possibly deadlier, Novavax reported that its vaccine seemed to be nearly as effective at preventing illness from the variant as other circulating strains (95% effectiveness vs 85%).
The company also presented data from a Phase 2b trial in South Africa, where the more transmissible variant B.1.351 has been spreading widely. The vaccine was deemed to be 60% effective at preventing any illness from the virus in HIV-negative people (across both HIV-positive and HIV-negative volunteers, the efficacy was 49%). And when they studied covid-19 positive cases more closely, nearly all of those identified were caused by B.1.351.
On Friday morning, Johnson & Johnson announced results from preliminary trial data of its candidate, which is being tested out as a single-shot treatment (currently approved covid-19 vaccines in the U.S. require two shots a month apart). Overall, it was shown to be 66% effective overall in preventing moderate to severe illness from the virus, but there were varying levels of effectiveness in different parts of the world. In the U.S., the effectiveness was 72%, but in South Africa, it dropped to 57%, which is likely due to the prevalence of B.1.351 in the country.
These trial results for Novavax and J&J aren’t quite as rosy as they were for Pfizer/BioNTech and Moderna’s vaccines, which were the first two to win approval in the U.S. and Europe late last year and are both based on similar mRNA technology (both have shown around 95% effectiveness against illness, though this data was obtained before the emergence of the new variants). But even if these second-wave vaccines are less effective, that doesn’t mean they wouldn’t be valuable tools in fighting off the pandemic.
Both the Novavax and J&J vaccines can be stored in standard refrigerator temperatures (between 36° and 46° Fahrenheit), unlike the Pfizer/BioNTech vaccine, which requires extremely cold temperatures. Moderna’s vaccine can be kept in a refrigerator for up to 30 days, but it is still highly sensitive to lighting and temperature changes once taken out. Both of the newer vaccines are also expected to be cheaper than the mRNA vaccines, which will likely be a crucial factor for lower-income countries that are facing hurdles in securing enough vaccines for their residents. J&J’s vaccine, being a single shot, would allow for smoother distribution as well. That said, there are trials of a two-dose formulation ongoing, which could show that a booster shot will improve its effectiveness.
Perhaps most importantly, though, is that these vaccines are likely still highly effective at preventing severe illness and death from covid-19, even from the new virus variants. Novavax’s results found no severe cases among vaccinated people who developed illness. And J&J’s candidate was found to be 85% effective overall at preventing severe illness, while no virus-related hospitalizations and deaths were found in the vaccinated group 28 days after treatment. A vaccine that protects more than half of everyone from illness and nearly everyone from serious complications is still one that would help turn the tide of the pandemic, even if the mRNA vaccines didn’t exist. Countries in Europe are already facing the prospect of shortages of the existing Pfizer/BioNTech vaccine, so any additional approved candidates would help.
That need is likely one reason why the EU has just today approved the emergency use of another vaccine, one developed by Oxford University and AstraZeneca. Their two-dose vaccine has shown to be around 60% effective at preventing illness overall (some mixed data has shown it to be more effective under a different dosing regimen, but that’s still uncertain). Of all the vaccines reaching the end of development, Oxford/AstraZeneca’s candidate is thought to be the cheapest to produce. The vaccine was previously approved in the UK late last December, along with the Pfizer/BioNTech vaccine.
Novavax has already submitted an emergency use authorization in the UK and is expected to file for one in the U.S., though likely not until its 30,000-person trial in the U.S. and Mexico is concluded. J&J is expected to submit its vaccine for an emergency use authorization in the U.S. in early February, and a decision may arrive within two weeks, according to Anthony Fauci, director of the U.S. National Institute of Allergy and Infectious Diseases. Oxford/AstraZeneca’s version may not be submitted for authorization in the U.S. until the spring, with a large-scale trial in the U.S. still ongoing.
In any case, it’s likely that several more covid-19 vaccines will be available to the world in the months to come. In the meantime, continuing to take precautions like wearing masks and avoiding large indoor gatherings will be crucial to saving lives and reducing strain on the healthcare system.