New outbreaks of a seldom-seen disease called monkeypox are setting public health experts on edge. Several countries, including the U.S., have recently reported cases of the viral infection. No deaths are reported so far, and the risk to the general public appears to be low for now. But it’s possible something has changed in the virus, or its relationship to humans, that’s making it more transmissible.
Officials at the World Health Organization announced the week of June 15that they will choose a different name for the disease, one that is intended to avoid the stigmatization and inaccuracy of its current moniker.
Countries with reported monkeypox cases
The first U.S. case involved a Massachusetts resident who recently traveled from Canada, where there have been 13 suspected cases. On late Thursday afternoon, New York City health officials reported a suspected monkeypox case, who is currently being treated at Bellevue Hospital. As of September 8 there have been 21,000 confirmed cases in the U.S.
At least 70 countries, including the UK, Canada, Spain, Portugal, Italy, Sweden, and the U.S. have documented cases of monkeypox. In the UK, the first reported case is believed to have contracted it while in Nigeria. Australia reported its first case Thursday, in someone who had recently traveled from the UK. Germany, France, and Belgium reportedtheir first cases Friday morning. There are now believed to be around 15,000 reported cases worldwide.
On May 20 the World Health Organization announced it will hold an emergency meeting over monkeypox, where experts will deliberate over whether to declare the outbreaks a Public Health Emergency of International Concern (PHEIC). The last such major and ongoing outbreak to receive PHEIC status is the covid-19 pandemic.
The first human cases of monkeypox were documented in Africa in the 1970s, and it’s been occasionally spotted on the continent since then. But it’s a zoonotic disease, meaning that infections are usually transmitted from animals to humans (despite the name, rodents are thought to be the primary vector) rather than between people. So these multiple outbreaks in several countries, with evidence of local transmission in some, are very different from what we’ve seen before, according to Andrew Pavia, an infectious disease doctor at the University of Utah. But there’s no clear answer yet as to why this is happening, he adds.
“In the past, human to human spread has occurred but has been quite limited. We don’t know that it is spreading more easily from person to person yet. That is one possible explanation, but I am not aware of any evidence to support that idea yet,” Pavia told Gizmodo in an email.
What is monkeypox virus?
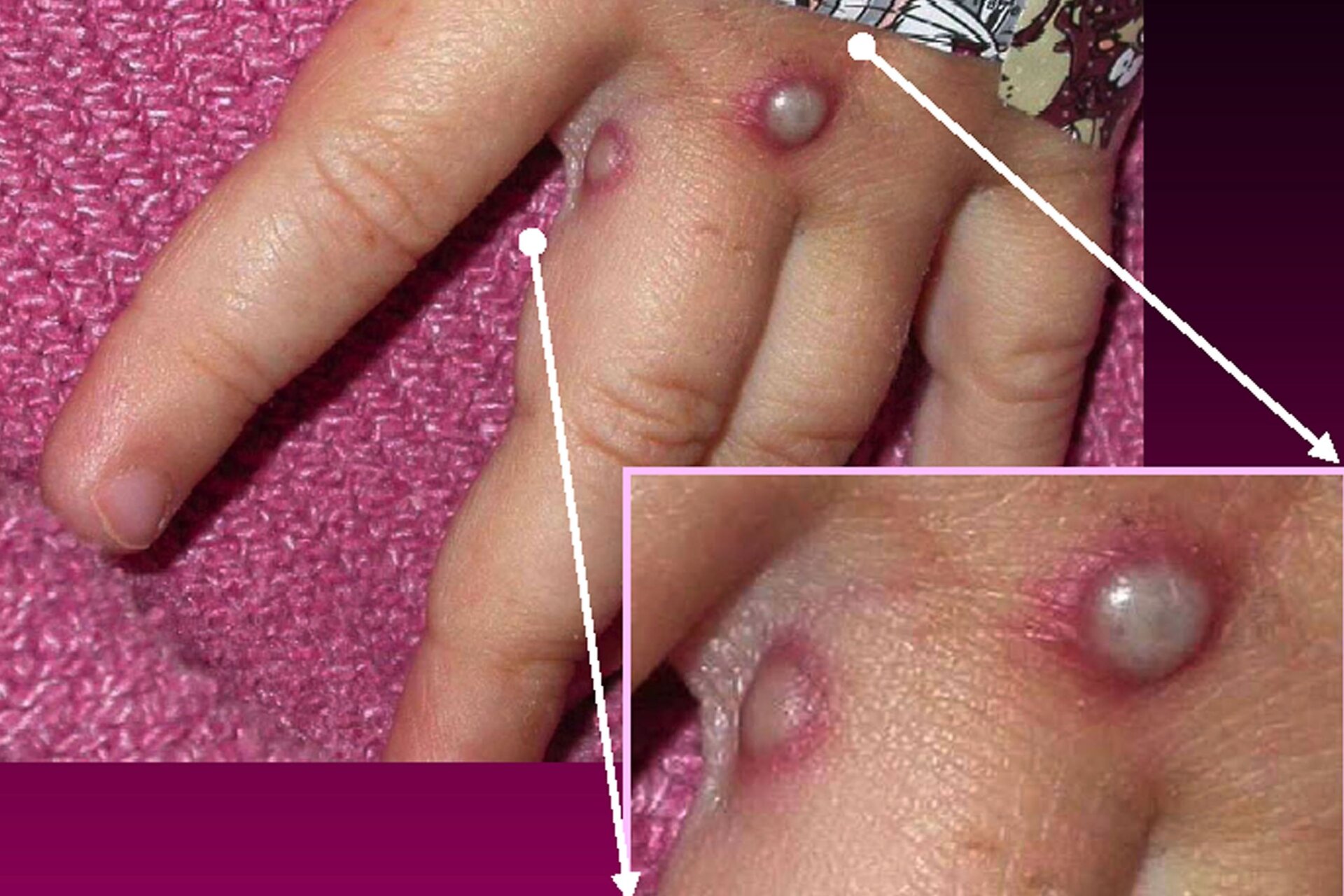
Monkeypox is caused by its namesake virus, a member of the poxvirus family. It’s a close cousin to the smallpox virus, the only human germ so far to be fully eradicated. Like smallpox, monkeypox infection causes distinct bumpy rashes that usually start in the face and spread throughout the body, along with flu-like symptoms.
It takes one to three weeks following exposure for symptoms to begin, and people are usually sick for about two weeks. As many as 10% of victims can die from it, though the cases documented in the UK appear to be caused by a lineage of the virus known to be less virulent, with a fatality rate closer to 1%. Though there are no deaths reported so far.
There are available tools against monkeypox that we could use if these outbreaks expand to become a greater threat. Smallpox vaccines should remain protective against monkeypox and can be given after exposure to prevent illness, so they can be used as a part of a “ring-vaccination” strategy to short-circuit outbreaks. There are approved antivirals that have shown effectiveness against poxvirus infections, as well.
Why is monkeypox spreading now?
A few researchers have been able to genetically sequence samples of the virus from some patient. The results suggest that the strain in these cases are actually closely related to strains that were recently collected from Nigeria, where outbreaks have been occurring since 2018. However, there does not seem to be evidence that the virus has mutated in a significant way since then. Further research is necessary to rule out the possibility that it somehow become more contagious between people
But some scientists like Jo Walker, an infectious disease epidemiologist and modeler at the Yale School of Public Health, have speculated that this seemingly increased spread could actually be related to our victory over smallpox decades ago.
Smallpox was declared eradicated in 1980, through the efforts of a global mass vaccination program that created a wide net of population immunity. Poxviruses are known for causing cross-immunity to other related viruses (indeed, the weakened virus in the classic smallpox vaccine isn’t even smallpox). And this buffer of smallpox immunity may also have hampered monkeypox from spreading in humans. As time has gone by, though, our collective protection has waned over time for various reasons, perhaps allowing monkeypox to finally spread more widely, without needing to change in any important way.
“This ‘declining immunity’ is less due to waning immunity at the individual level, and more due to people with immunity dying, and people without immunity being born and then staying non-immune,” Walker told Gizmodo in a Twitter message.
Walker notes that some researchers have long warned about monkeypox or similar viruses someday filling in the niche left behind by smallpox, and some have argued that it’s a major factor in why the germ made a reappearance in Nigeria starting in 2017, following four decades of zero reported cases.
Another possibility Pavia brings up is that some mystery animal has played an outsized role in seeding these outbreaks. In 2003, he points out, the largest known but still small outbreak of monkeypox in the U.S. (47 cases in total) was traced back entirely to contact with infected pet prairie dogs—an unknown vector back then.
At the same time, there is evidence of human-to-human transmission in at least some of these cases. In the UK and Spain, the majority of cases have been found in young gay and bisexual men, raising the possibility that these infections were sexually transmitted, with one World Health Organization adviser making the argument that the spread may have been amplified by two recent raves in Spain and Belgium where casual sex was common. Even if this is true, it does not mean that gay and bisexual men are the only people at risk, since the virus can spread through direct contact between any sex partners. Other research has suggested that monkeypox can theoretically survive in the environment in aerosol particles intact enough to be considered airborne.
Getting to the bottom of this monkeypox mystery will require classic medical detective work, Pavia said. Epidemiologic investigations will try to figure out the type of contact that resulted in people’s infections and the number of infections that seem to spring up from each index case. In the lab, scientists will be looking for possibly relevant genetic changes in the virus samples taken from patients, or testing out whether these infections behave differently in model animals.
“Given what we know today, there is no reason to panic or for most people to have any worries, but it is early days, so that may change,” Pavia said.
This article has been updated as of September 8 with the latest case count.






