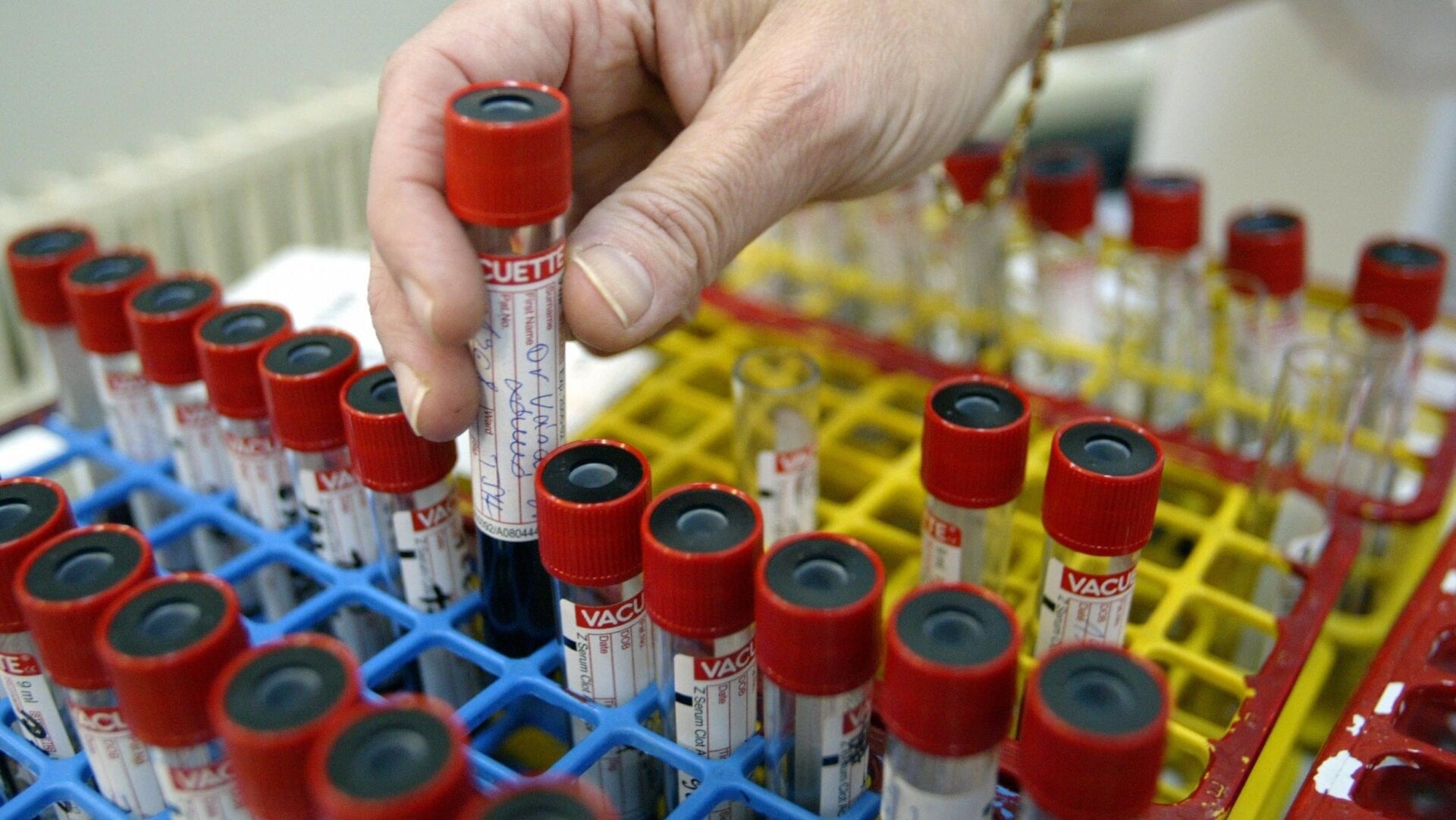
New research indicates that over 80% of American adults now have antibodies to the coronavirus, earned either through infection or vaccination. The study, based on data collected from blood donors, estimates that over 80% of Americans over the age of 16 had these antibodies as of May 2021. The authors do caution, however, that their results may not be generalizable to the entire U.S. population.
The study, published Thursday in JAMA, is the work of researchers from various blood donation organizations as well as the Centers for Disease Control and Prevention’s pandemic response group.
Every month starting in July 2020, the team has been analyzing samples of donated blood collected from people over 16 in the U.S., looking for antibodies specific to covid-19. The samples were taken from all 50 states, from areas representing about 74% of the country’s population. After the vaccination campaign began in December 2020, the team added a second test to differentiate positive antibody results as either infection- or vaccine-induced (both vaccination and infection compel the body to produce antibodies to the virus’ spike protein, but infection also generates a response to other parts of the virus). By May 2021, they had collected just under 1.5 million blood specimens.
Using these samples as a baseline, they estimated that 3.5% of Americans over age 16 had antibodies to the virus by July 2020, all through being infected. By May 2021, the percentage of Americans with these infection-induced antibodies was estimated to be 20.2%. And when combining both types of immunity, they estimated that 83.3% of adults had antibodies overall.
“Based on a sample of blood donations in the US from July 2020 through May 2021, vaccine- and infection-induced SARS-CoV-2 seroprevalence increased over time and varied by age, race and ethnicity, and geographic region,” the authors wrote.
The results come with some important limitations. People willing to donate blood may be different from the general public in relevant ways that could have affected their likelihood of getting infected or later getting vaccinated. And because you have to be over 16 to donate blood in the first place, this can’t tell us anything about the prevalence of antibodies in younger people. Antibody tests aren’t flawless, either, and some unlucky people may not generate detectable antibodies following infection or vaccination, while antibodies in some may wane to undetectable levels over time (though the jury is still out on how often either happens). Immunity is also more complicated than simply having the right antibodies.
Lastly, since the end of May, there have been millions more people vaccinated or infected, meaning the team’s estimate is likely lower than the true current percentage of American adults with antibodies.
The authors did try to account for possible differences between blood donors and the general public in coming up with their estimates. But they acknowledge that their math could have come up short.
“Despite weighting to adjust for demographic differences, these findings from a national sample of blood donors may not be representative of the entire US population,” they wrote.
Given all this, these numbers should be taken as a rough sketch of our collective immunity to the coronavirus, not an exact figure. But they do show that vaccines have greatly sped up the process of Americans having some degree of immunity to the virus, while offering highly effective protection against the worst outcomes of coming face to face with covid-19. The risk of hospitalization, death, and even long-term symptoms is substantially lower in the vaccinated than in the unvaccinated and unexposed. Unfortunately, the results also suggest that there are still millions of Americans at risk of contracting the virus with no preexisting immunity at all.
The team plans to keep tracking the prevalence of coronavirus antibodies among blood donors until December 2021.