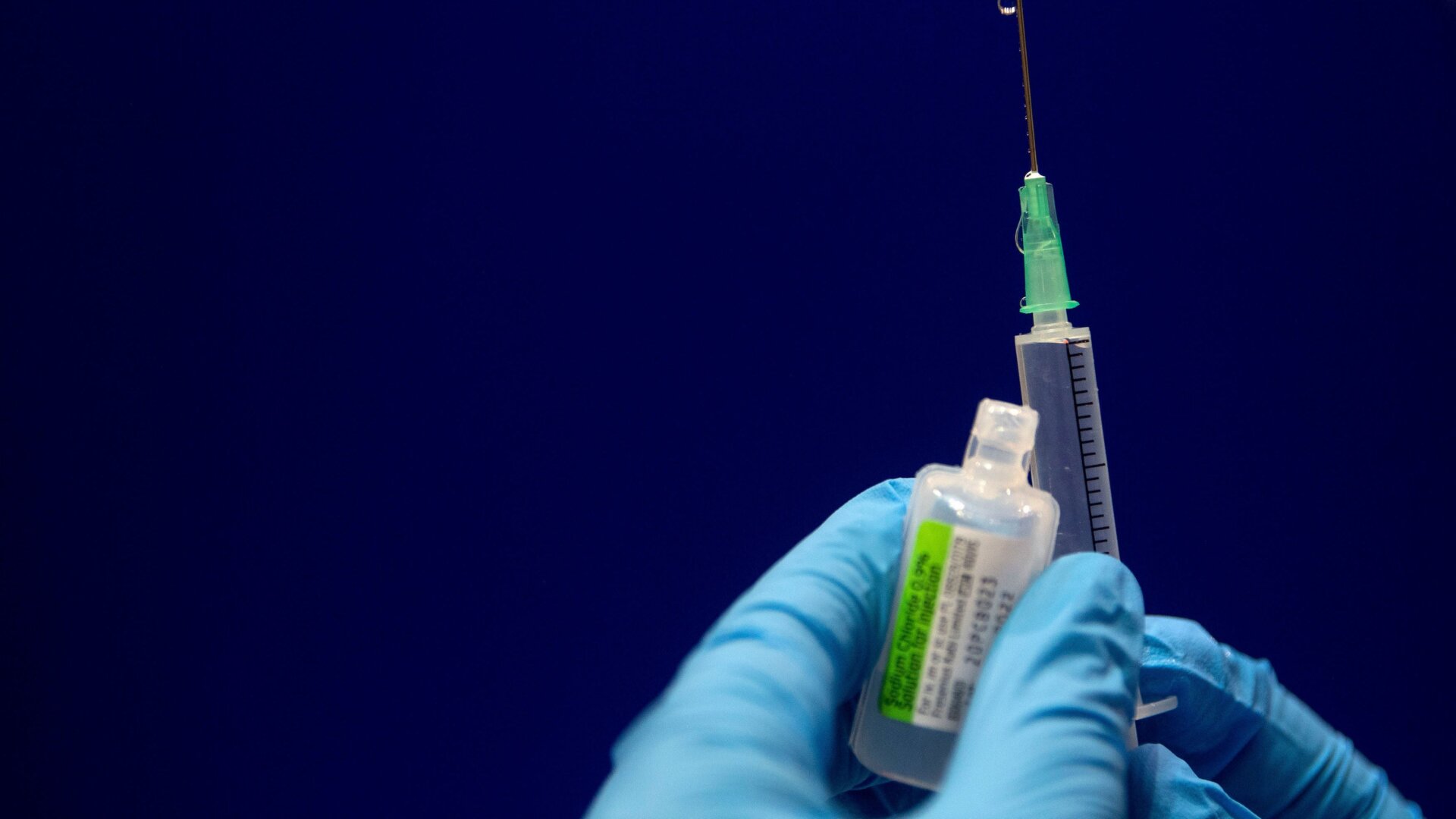
On Friday, the Food and Drug Administration granted an emergency use authorization to the covid-19 vaccine developed by Pfizer and BioNTech, making it the first vaccine against the viral pandemic that will reach the American public. The decision was expected and came soon after a group of outside experts assembled by the FDA voted to recommend its use.
The approval reportedly came after White House Chief of Staff Mark Meadows put pressure on the agency and told FDA Commissioner Stephen Hahn to start looking for another job if he did not authorize the vaccine by day’s end on Friday, sources familiar with the matter told the New York Times and the Washington Post under the condition of anonymity. The FDA was originally planning to issue formal authorization of the Pfizer/BioNTech vaccine, which is administered as a series of two doses, three weeks apart, on Saturday morning. However, the expedited timing of the announcement isn’t expected to speed up the delivery of vaccines nationwide, which is likely to begin within the coming days.
The FDA issued the following statement on Friday:
“Following yesterday’s positive advisory committee meeting outcome regarding the Pfizer-BioNTech COVID-19 vaccine, the U.S. Food and Drug Administration has informed the sponsor that it will rapidly work toward finalization and issuance of an emergency use authorization. The agency has also notified the U.S. Centers for Disease Control and Prevention and Operation Warp Speed, so they can execute their plans for timely vaccine distribution.”
Hahn called the authorization “a significant milestone in battling this devastating pandemic that has affected so many families in the United States and around the world,” and commended how quickly a covid-19 vaccine was developed, calling it “a true testament to scientific innovation and public-private collaboration worldwide.”
The pivotal data used to evaluate the vaccine came from a still ongoing large phase III double-blinded, placebo-controlled, and randomized trial involving more than 44,000 volunteers in the U.S. age 16 or older. In this trial, the two-dose vaccine appeared to be 95% effective at preventing symptoms of covid-19 a week after the second dose was received. Adverse effects more commonly seen in people vaccinated included injection site pain, fatigue, fever, and headache.
https://gizmodo.com/pfizers-covid-19-vaccine-wins-crucial-vote-now-one-ste-1845855119
Despite the good news, there are many logistical and scientific questions left to be answered about the vaccine. The FDA still plans to evaluate the vaccine for a full approval, which will require longer data collection on its effectiveness and safety.
“While not an FDA approval, today’s emergency use authorization of the Pfizer-BioNTech covid-19 vaccine holds the promise to alter the course of this pandemic in the U.S.,” Peter Marks, M.D., Ph.D., Director of the FDA’s Center for Biologics Evaluation and Research, said in a statement.
Pfizer has stated its preference to vaccinate those who received the placebo during the trial, but experts are worried that this will hamper attempts to study the longer-term outcomes of people originally vaccinated, since there would no longer be a control group for comparison.
One potential compromise, discussed during the advisory committee meeting held Thursday, is to allow people in either group to receive the extra doses, but only as they become eligible to receive it. Those given the vaccine originally would only receive a placebo, while those who received a placebo would be given the vaccine. This would effectively keep the study blinded, and still allow scientists to compare their outcomes over time in some ways.
There are also other possible risks that scientists and public health agencies like the Centers for Disease Control and Prevention will be keeping an eye out for. For instance, four vaccinated people in the trial developed Bell’s palsy, a usually temporary condition where facial muscles become droopy or paralyzed, while no people in the control group did. It’s possible this could be a real side effect of the vaccine, but the rate of Bell’s palsy seen in the vaccine group was no greater than the rate seen in the general population, so it may have only been a coincidence. There were also reports of two people with a history of allergies in the UK developing a serious allergic reaction after they took the vaccine this week, which prompted a new warning by the country’s health regulator. It’s almost certain the CDC will be tracking that potential risk as well.
Another question is whether Pfizer and BioNTech’s vaccine (as well as Moderna’s similar mRNA vaccine) can prevent asymptomatic cases of covid-19 as well, which would be important for preventing transmission altogether. If vaccinated people can still carry a silent infection, then they risk spreading it to other unvaccinated people. However, during the meeting Thursday, Pfizer stated that it would have the data needed to know the answer to this question sometime early next year.
The emergency use authorization, or EUA, will allow the vaccine to be used for Americans over the age of 16. The EUA doesn’t dictate who should receive the vaccine first, however, nor is the FDA the only health agency involved in sanctioning its use. Over the weekend, the CDC’s Advisory Committee On Immunization Practices (ACIP) met to discuss the vaccine data, as well as offer their own recommendations for the vaccine’s eligibility.
Earlier this month, the ACIP decided on interim guidelines for any covid-19 vaccine’s initial eligibility, stating that health care workers and elderly residents in long-term care facilities should receive the first batch of doses available.
Even with the Pfizer/BioNTech vaccine’s authorization, there’s still the looming challenge of getting doses to as many vulnerable Americans as quickly as possible, especially in the face of a resurgent pandemic that is now killing more people in America than ever; more than 3,000 daily deaths were reported on Wednesday and Thursday.
Though the ACIP’s guidelines for who should get the vaccine first will be followed closely by states, they each have their own individual distribution plan. There are concerns that even frontline health care workers will not have access to the vaccine in more remote areas of the country until next year. There are also only so many doses to go around, with Pfizer estimating that a maximum of 20 million will be available to the U.S. by the end of the year. Moderna’s vaccine candidate, which will be evaluated by the FDA next week, is in similarly short supply this year should it be given its own EUA.
These are all valid concerns. But we shouldn’t forget the monumental scientific accomplishment on display here either. Assuming Moderna’s vaccine is authorized for use, the country will have two highly effective vaccines for a newly discovered disease developed in less than a year’s time, breaking the previous record for getting a vaccine to market by years. Over the next few months, these and possibly other vaccines will help humanity defeat the deadliest pandemic seen in over a century—all thanks to the tireless efforts of scientists and the bravery of ordinary citizens who volunteered to test them out.
This story includes additional reporting from Alyse Stanley.