The growing use of Ozempic and other GLP-1 drugs has had an outsized, sometimes negative, impact on all sorts of industries, particularly those related to food. Another such casualty, research out today suggests, seems to be weight loss surgery.
Researchers examined a major database of bariatric surgeries performed in the U.S. Following a rise in recent years, the estimated number of total procedures took a sharp dive in 2024, they found. Though the study can’t show the cause for this decline, the researchers suspect that GLP-1s are playing a big part. They also worry some people with severe obesity are being steered away from the surgical treatments they would most benefit from as a result.
“Our concern with the current state of obesity treatment is that the marketing of GLP-1 medications and their massive popularity is overshadowing scientific evidence supporting metabolic and bariatric surgery as the most efficacious therapy for obesity,” lead study author Tyler Cohn, a surgeon and associate professor at Loyola University Medical Center, told Gizmodo.
The GLP-1 crunch?
Semaglutide is the active ingredient in Ozempic and Wegovy (Ozempic is approved for type 2 diabetes, whereas Wegovy is approved for obesity). It mimics the GLP-1 hormone, which helps regulate our hunger and insulin production. The latest GLP-1 drugs like semaglutide are much more effective at helping people lose weight than diet and exercise alone, as well as most other weight loss interventions. The glaring exception to that, even today, are the most commonly performed bariatric surgeries, the gastric bypass and the sleeve gastrectomy.
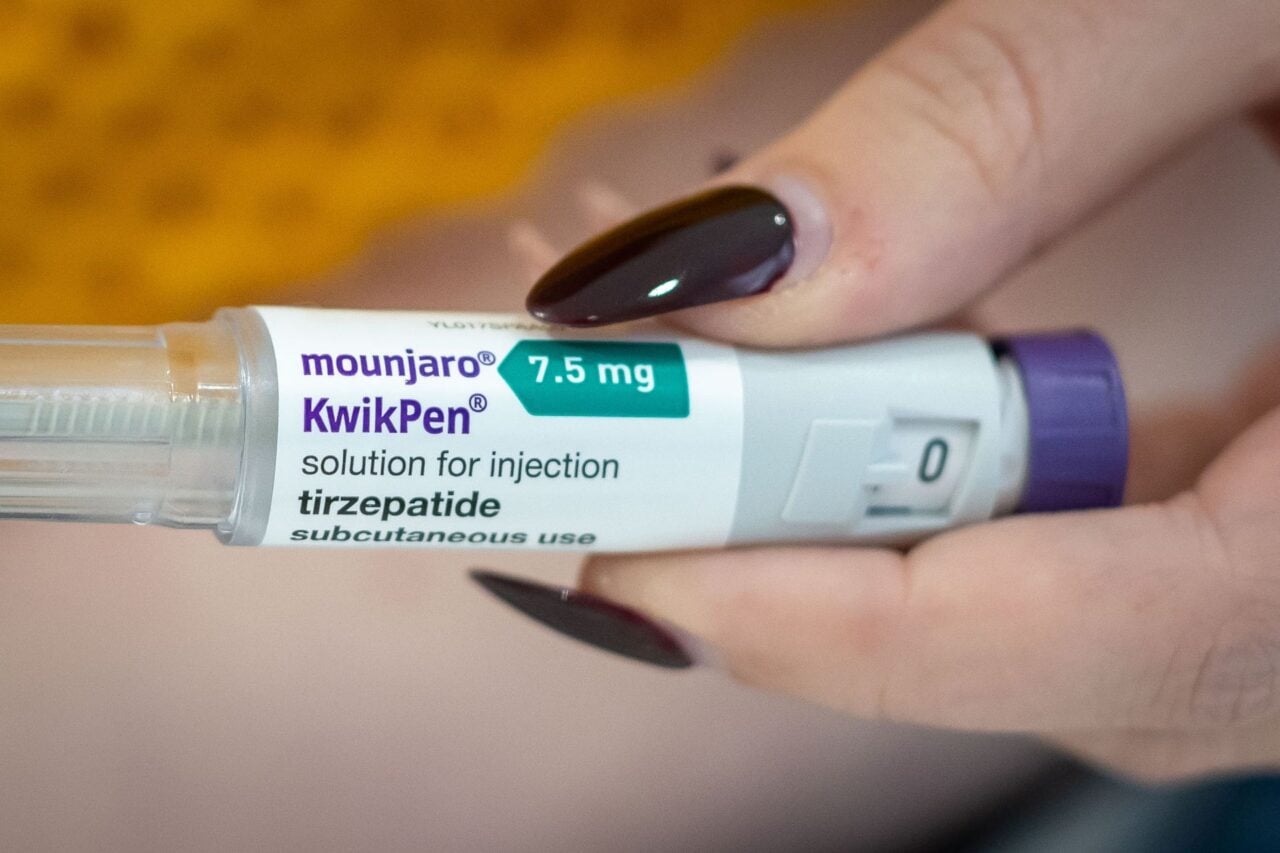
People who undergo these surgeries typically lose between 25% and 35% of their baseline weight in the first year (sleeve gastrectomy patients are usually on the lower end of that range), compared to the average 15% weight loss seen with Wegovy. Newer GLP-1 iterations that target multiple hormones like tirzepatide can cause more weight loss, though it still tends to come up a bit short compared to surgery (around 16% to 22%).
In addition to providing more weight loss on average, studies have also found that bariatric surgery is more cost-effective, particularly for people with the most severe cases of obesity. And many people might not be able to tolerate the likely lifetime upkeep of GLP-1 therapy, compared to a single surgery.
Researchers at Loyola University in Chicago sought to examine bariatric surgery trends in the wake of the GLP-1 era. They analyzed data from the American College of Surgeons Metabolic and Bariatric Surgery Accreditation and Quality Improvement Program (ACS-MBSAQIP), which tracks surgeries performed at all MBSAQIP-accredited centers. Based on this data, the researchers estimated how many bariatric surgeries were performed in the U.S. between 2020 and 2024.
Bariatric surgeries, like many medical procedures, are known to have declined during the first full year of the covid-19 pandemic in 2020. The researchers found that surgeries then increased over the next couple years, reaching an estimated peak of 230,207 procedures in 2022. After that, however, they started dropping. There were only an estimated 177,297 procedures performed in 2024, a 23% decrease relative to 2022 and the lowest number since 2020.
About 58% of surgeries in 2024 were sleeve gastrostomy, a drop from 64% of all surgeries in 2020, while 33% of surgeries in 2024 were gastric bypass, up from 28% in 2020. Some patients also undergo additional procedures to modify or revise their initial surgery. According to the study, 11% of bariatric procedures in 2024 were these secondary conversions, compared to 9% in 2020.
GLP-1s have genuinely changed the world of obesity treatment for the better, but some people with severe obesity might be turning down surgery when it’s likely to be their best course of action, the researchers say.
“The most important takeaway for the public is to understand that metabolic and bariatric surgery has evolved over many decades to be a safe and highly effective therapy for severe obesity that results in durable long-term weight loss for the vast majority of patients,” Cohn said. “Surgery results in greater weight loss and lower healthcare costs than GLP-1RA therapies with proven long-term results.”
The team’s findings are being presented this week at the annual scientific meeting of the American Society for Metabolic and Bariatric Surgery (ASMBS). The study is also expected to be published in the peer-reviewed journal SOARD, though a publication date is still pending.
What might this mean for obesity patients?
It’s possible that the researchers underestimated how many surgeries are carried out annually. According to the ASMBS, which bases its estimates on multiple datasets, not just the ACS-MBSAQIP, there were over 270,000 bariatric procedures performed in 2023 (the latest year available). Still, other research has shown that weight loss surgeries are generally on the wane. And though these studies alone can’t prove that GLP-1s are the culprit, there’s solid circumstantial evidence behind the notion.
A peer-reviewed study published earlier this March, for instance, found that prescription rates of semaglutide and tirzepatide started rising substantially toward the end of 2022, while rates of bariatric surgery began dramatically declining in 2023. Notably, while Wegovy was first approved in June 2021, high out-of-pocket costs, sparse insurance coverage, and factory-related shortages likely limited how many eligible people could obtain these medications early on, which might help explain the delay in declining surgery rates.
The calculus of GLP-1 therapy compared to surgery is likely to change over time. The out-of-pocket costs of GLP-1s have significantly lowered as of late, and this year, cheaper generic versions of semaglutide are launching in both Canada and India (unfortunately, Americans will have to wait until 2032 for the same). Experimental drugs that might match the average weight loss seen with surgery are also now in late-stage development and could reach the public by next year.
In an ideal world, both GLP-1s and surgery will continue to be important obesity treatments that can even be complementary to each other. Some studies have found evidence that GLP-1 use before surgery can reduce post-operative complications for people with extreme obesity, for instance, while GLP-1s after surgery might help some avoid weight regain.
Importantly, many people with obesity still aren’t getting any treatment at all. According to the ASMBS, less than 1% of people eligible for bariatric surgery receive it in any given year. And though more than 40% of Americans under 65 with private insurance are likely eligible for GLP-1 medications, only about 12% of adults are currently taking one.
“Metabolic and bariatric surgery is not right for everyone but warrants consideration for those who qualify,” Cohn said. “Patients seeking treatment for obesity should learn about all their options prior to selecting a therapy.”
The researchers plan to continue exploring this topic, which will include studying the reasons why patients might choose the obesity treatments that they do.